Program Explain Pain Butler Moseley Pdf To Word
Explain Pain (by the sea) A TWO-DAY INTERACTIVE SEMINAR Based on and expanding Butler and Moseley’s book, ‘Explain Pain. COURSE PROGRAM DAY ONE: 8.30 - 5pm. The evidence base for ‘Explain Pain’ Authors David Butler and Dr Lorimer Moseley, ISBN 0 9750910 Published by Noigroup Publications, Adelaide, South Australia Introduction There are a number of dimensions to evidence. Everyone, when injured or in pain wants to know what is wrong and how long the problem will last. It is self evident. Pain is multidimensional and requires attention to the emotional and psychosocial. British Pain Society (2007) Recommended Guidelines for Pain Management Programmes for Adults. Butler DS, Moseley L (2008) Explain Pain. Available at www.citra.org/Assets/documents/pain%20conference%20summary.pdf.
Noigroup Publications, Adelaide, Australia, 2003 19 North Street, Adelaide City West, South Australia 5000
1
----------1
Published by Noigroup Publications for
Noigroup Publications
NO! Australasia, Pty Ltd.
NO! Australasia Pty Ltd 19 North Street, Adelaide City West,
Printed and bound by Nexus Print Solutions,
South Australia 5000
Adelaide, South Australia.
www.noigroup.com Telephone +61 (0)8 8211 6388
Copyright 2003 Noigroup Publications.
Facsimile +61 (0)8 8211 8909 [email protected]
All rights reserved. No part of this publication may be reproduced, stored in a retrieval system or
Butler, David S. and Moseley, G. Lorimer
transmitted in any form or by any means, electronic,
Explain Pain
mechanical, photocopying, recording or otherwise,
First edition 2003
without the prior written permission from the
First reprint 2004
publisher, except for brief quotations embodied in
Second reprint 2006
critical articles and reviews .
Third reprint 2007 Includes index
The procedures and practices described in this book should be implemented in a manner consistent with professional standards set for the circumstances that apply in each situation. Every effort has been made
ISBN 09750910 0 X 9 780975 091005 C)
to confirm accuracy of the information presented and
National Library of Australia
to correctly relate generally accepted practices.
A catalogue record for this book is available from the National Library of Australia
The authors, editor and publisher cannot accept responsibility for errors or exclusions or for the
State Library of South Australia
outcome of the application of the material presented
A catalogue record for this book is available
herein. There is no expressed or implied warranty of
from the State Library of South Australia.
this book or information imparted by it.
Acknowledgments Many people help in the production of a book, especially when it is self published. We both want to give special thanks to Ariane Allchurch for her great design work, typesetting, graph construction and transforming the pile of pages and images into a book. Special thanks to Anna Bianchi, Anna Hill and Jane Barrett for proofreading. Thanks to Sunyata for his unique artwork, zeal and skill in turning concepts into powerful and sometimes poignant graphics. Thanks to the anatomy department at the University of Adelaide for the use of cadaver material. Very special thanks and much gratitude to Juliet Gore, general manager of Noigroup for keeping the project going, realising its importance to us and to patients and always having the end vision. Thanks to the wonderfully supportive Noigroup team: Anna Bianchi, the pivotal person of the office, Rob Dick for website support, Frank Navacchi for office equipment, Wendy Tims for organisational direction and office humour, Neville Andrigo for environmental protection, Dinah Edwards for design advice and Dick Murn for keeping the rain out of the office on most occasions. Thanks also to Peter Vroom for his help with budgeting and to Danny Beger for legal support. We wish to thank the Noigroup teaching team for their L contributions and help in spreading the message. Adriaan Louw, Bob Nee, Bob Johnston, John Tomberlin, Peter Barrett,
Carolyn Berryman, Megan Dalton, Hannu Luomajoki, Hugo Stam, Martina Egan-Moog, Michel Coppieters, Gerti Bucher-Dollenz, Harry von Piekartz and Irene Wicki. Thanks to the many students we have taught in many countries. Our shared experiences and their desire to learn have added richness and depth to this book. And special thanks to the many people in pain who have told us their stories and shared with us their fear and liberation. From David: thanks to David Mallett and Margaret Stuart, neighbours extraordinaire, for looking after us and the cat while we worked into the night . Lots of love and many thanks to Juliet . You really did keep it and us together. From Lorimer: thanks to Paul Hodges who taught me that scientific rigor is not what happens when you die. Thanks to the Kaboobies, from whom I first learnt that to love and to be loved is what it is all about. Finally (as always!) to Anna Hill - you are superb! As in all you do, you are here. We dedicate this book to Professor Patrick Wall (1925-2001) who encouraged us both to take the road less travelled, to fight the creeping forces of blinded peripheralism and scientific arrogance and to regard the patient always as a person. It is our greatest wish that he could have enjoyed this book.
Lorimer and David Australia, July 2003
Section 1 8 10 12 14 16 18 20 22 24
Introduction Pain is normal Amazing pain stories Part 1 Amazing pain stories Part 2 Amazing pain stories Part 3 Pain relies on context Part 1 Pain relies on context Part 2 The phantom in the body Age, gender, culture and pain
Section 2 28 30 34
36 38
40 42
Introduction: Your remarkable danger alarm system A closer look at alarm signals Sending messages The alarm message meets the spinal cord The message is processed throughout the brain The orchestra in the brain Systems to get you out of trouble
Section 3 46 48 50
52 54
56 58
60 62 64 66
Introduction: The damaged and deconditioned body Acid and inflammation in the tissues Inflammation: The brain is immediately interested The truth about muscles Get to know your LAFTs Get to know your skin and soft tissues Bone and joint contributions to pain The peripheral nerves The dorsal root ganglion - the peripheral nerve's minibrain Backfiring nerves What you might notice with nerve pain
Section 4 70 72 74 76 78 80 82 84 86 88 90
Introduction: Altered central nervous system alarms Altered central nervous system alarms - the spinal cord The spinal cord as a magn1f:l.er of tissue reality The brain adapts and tries to help The orchestra plays the pain tune Thoughts and beliefs are nerve impulses too The sensitised central alarm system Response systems - the sympathetic and parasympathetic nervous system The endocrine response The immune system Movement strategies
Section 5 94
Introduction: Modern management models
96 98 100 102
Models of engagement Part 1 Models of engagement Part 2 Fears associated with movement and pain Coping with life and pain
104
Your relationship with pain
Section 6 108 110 112 114 118
Introduction: Management essentials Tool 1: Education and understanding Tool 2: Your hurts won't harm you Tool 3: Pacing and graded exposure Tool 4: Accessing the virtual body
125 128 129
References Index Further reading
Use of this book This book has four aims . First, to assist a variety of
The principles presented in this book are particularly
health professionals in explaining pain, we wanted to
suited to consideration of chronic non -specific pains
provide a conduit from the world of basic neuroscience
(e.g. low back pain, elbow pain). However, they can be
to clinicians and to their patients. Second, to enable
extended to pain states such as rheumatoid arthritis and
people in pain to understand more about their situation
used in conjunction with other management strategies.
and to become less frightened of their pain. We know that the threat value of pain contributes directly to the
We think that one strength of this book is that anyone who
pain experience and by informing people about what is
suffers from persistent pain, or has a loved one, colleague
actually happening inside them we can reduce the
or friend who has persistent pain, can directly benefit
threat. Third, to assist people in pain, and those
from using the book. The benefit will be greater with
involved with them, to make the best choices about their
guidance from an informed clinician where necessary.
management. Finally, to outline modern models of management and provide the management essentials for
Finally, it is hoped that health professionals will find
overcoming pain and returning to normal life.
this book, and the view of pain and pain management that is presented, helpful as they try to integrate
The book is designed so that it can be used as a manual
modern pain SCience into therapy. Every effort has been
for clinicians to explain pain to patients, as a workbook
made to reference the material with up-to-date and
completed by patient and clinician together, as part of a
relevant scientific literature. The literature in this area
cognitive-behavioural/multidisciplinary pain
is vast so we have selected the most representative
management programme, or for the patient to use as a
literature. There is also a list of relevant 'easyread'
'take-home' resource.
books on page 129.
You will find as you read, small numbers scattered
Lorimer and David
throughout the text. These relate to references for further reading or sources where we have found the information. The references are listed in numerical order on page 125.
• • • • • • • • • • • • • • • • • • • • • •
•
9
Most commonly, pain occurs when your body's alarm system alerts the brain to actual or potential tissue damage. But this is only part of a big story. Pain actually involves all of your body systems and all of the responses that occur are aimed at protection and healing. However, when most of us think of pain we think of the experience of pain - that unpleasant and sometimes downright horrible experience that makes you take notice and motivates you to do something about the situation. In fact, pain can be so effective that you can't think, feel or focus on anything else. If the brain thinks that experiencing pain is not the best thing for your survival (imagine a wounded soldier hiding from the enemy) you may not experience pain at the time of even very severe injury. There are many myths, misunderstandings and unnecessary fears about pain. Most people, including many health professionals, do not have a modern understanding of pain. This is disappointing because we know that understanding pain helps you to deal with it effectively. Here are two important things we now know about explaining pain: the physiology of pain can be easily understood by men and women in the street 1 , and understanding pain physiology changes the way people think about pain, reduces its threat value 2 and improves their management of it. Hopefully, you will find this journey as exciting, fascinating and empowering as we have. Read on ...
pain
1 10
Pain is normal It's sensible to have a system which protects and preserves
and may even become the topic of nursery rhymes (e.g. 'Norman's nose got bit by the chimp ... ever since then the chimp's had a limp, Norman's son knows dad is a whimp ... Poor old nosey Norman'). You get the message. You can have pain with much less obvious damage. It may just emerge over time as it has with the computer-bound Mr Lee. Pain is useful here and will hopefully encourage him to get up and move. But pain is often unpredictable, which can make us frightened of it. Sometimes you can lift an
Ofcourse things hurt; life can hurt. There
object a thousand times without a problem.
are many kinds of pain. In the unlikely
Then, all of a sudden, one lift causes
event that a monkey happens to bite your
extreme pain. Why would Sidney over the
nose, as it has bitten Norman's, then it will
page ever want to throw Rene Descartes'
hurt and you will probably remember the
bust into the bin again? By the way, Rene is
incident for the rest of your life - Norman
the French philosopher who invented the
probably won't show off like this to his son
mind-body split. There is no doubt that
next time they go to the zoo; the story of
Rene Descartes was extremely clever, but it
Norman's nose holes will be retold at
is 400 years since he proposed his theories.
countless family gatherings; it will change
We now know enough to be sure that this
the way the family thinks about monkeys;
mind-body split does not exist.
11 Pains from bites, postural pain and sprains are
If you are in pain right now, then you are not alone.
simple 'everyday' pains that can be easily related to
In fact, at any one time on the face of the earth,
changes in tissues. The brain concludes that the
around 20 percent of people have pain that has
tissues are under threat and that action is required,
perSisted for more than 3 months'. That's 2 million
including healing behaviours. An added benefit is
Londoners!
that memories of the pain will hopefully protect you from making the same mistake twice. Maybe the
When pain persists and feels like it is ruining
monkey bite nursery rhyme provides future
your life, it is difficult to see how it can be
protective behaviours for a whole family.
serving any useful purpose. But even when pain is chronic and nasty, it hurts because the brain
But we all know that pain can be a more complex
has somehow concluded, for some reason or
experience. The word 'pain' is also used in relation
another, often completely subconsciously, that you
to grief, loneliness and alienation. What is it about
are threatened and in danger - the trick is finding
the pain of lost love that makes it as debilitating as
out why the brain has come to this conclusion.
any acute low back pain? This emotionally laden pain helps us to grasp a big picture for understanding pain. All pain (in fact, all experiences!) involves many thoughts and emotional contributions. We need the brain in order to really understand pain especially pain that perSists, spreads or seems unpredictable. We need the brain to help us understand why emotions, thoughts, beliefs and behaviours are important in pain.
pain
1 12
Amazing pain stories Part 1
,
Some
P ain really is an amazing experience. Most of us have heard stories where people have had severe injury and no pain at the time of injury. AB the rat suggests - what happened to the warning system? Severe injury creates lots of loud alarm signals that pour into the brain, but these do not necessarily result in pain.
The amount of pain you experience does not
r
necessarily relate to the amount of tissue damage you have sustained. Look at Norman (still nursing his sore nose) with the arrow through his neck. While the monkey bite hurt a great deal, this comparatively serious injury may not hurt at all. In emergency rooms all around the world , patients present impaled by various objects. Many are lucky because the obj ect may not have interfered with vital organs and many report little or no paineg4 .
r
I
13 There are many stories from wartime. Take the World War II veteran who had some routine chest x-rays done. They revealed a bullet that had been lodged in his neck for 60 years - he never knew' . Many stories involve soldiers in wartime who have a severe injury, even losing a whole limb, yet who report little or no pain 6 • Those who suffered traumatic amputations in wartime and commented that there was no pain usually reported the injury in innocuous terms, such as a 'bump' or a 'thump,7. In other Situations, severely burnt people have run back into burning houses to save children; sportsmen and women have accomplished amazing feats despite severe injury.
But the ratio of the amount of injury to the amount of pain swings the other way too. What is it about a paper cut? It's not deep, there's not much damage, but it really hurts, it stings, it makes you annoyed and you can't believe that a paper cut could hurt that much. Obviously what's happening in your tissues is just one part of the amazing pain experience. Let's contemplate a few more amazing pain stories ...
pain
1 14
Amazing pain stories Part 2 The brain is obviously involved
L ow back pain and headache are among the most common pains in humans. In low back pain, research has shown that the amount of disc and nerve damage rarely relates to the amount of pain experiencedeg ,8. In fact many of us have scary sounding disc bulges, even squashed nerves, yet may never have any symptoms. We discuss this on page 61.
This can be a bit frightening, but it is really quite relieving. Many changes in tissues are just a normal part of being alive and don't have to hurt. What's more, these changes don't necessarily have to stop anyone leading a very functional and active life. It is very likely that an x-ray of an older person's spine will reveal changes which could be described as arthritic or degenerative, as you see in the yogi. They can still function very well.
Simply, if there is no pain it means that these changes in tissues are not perceived by your brain to be a threat.
15
Look at Sidney on his surfboard waiting for the perfect wave at Bondi Beach. Surfers who have had their legs bitten off by sharks have reported feeling nothing more than a bump at the time 9 •
(
We couldn't resist another common example of extreme forces on the body yet no complaints of pain. A football player who scores a significant goal is likely to have his
~ntire
team jump on him; a
weight of nearly a tonne. Yet he will always jump up Smiling and keep playing, often better than before. But under different circumstances a minor injury may be sufficient to lead a person into a life of chronic pain.
pain
1
16
Amazing pain stories Part 3
,
I
,
I
,
Even more intriguing
W hat about these true stories?
Pain is indeed complex. There is a well reported
Acupuncture can reduce pain, but it doesn't
syndrome called the Couvade syndrome, in
always work. In fact it is thought that
which the father experiences labour pain. In
acupuncture works best if it is performed by
some societies people believe that the more
a Chinese man on a Chinese woman in China
pain the father displays the better father he
and worst if it is performed by a non -Chinese
will be. Some wives actually look after the
woman, on a Chinese man, somewhere other
husband while delivering the childeg.1o,1l.
than China.
(
17
Hypnosis is fascinating. There are many records
shape of the tablet plays a part in the
of people who have undergone major surgery
effectiveness of the drug. Transparent capsules
while hypnotised, without medical anaesthesia 12 .
with coloured beads work better than capsules
How can this be? The alarm bells in the tissues
with white beads, which work better than
would still ring as the scalpel slices through
coloured tablets, which work better than
skin and muscle, yet there is no pain.
square tablets with the corners missing, which work better than round tablets 14 •
A little trivia - people around the world consume around 100 billion aspirin tablets per
Many and varied cues may relate to the
year. If you put them all in line, the line would
pain experience, but it is the brain which
be one million kilometres long (that's to the
decides whether something hurts or not,
moon and back yo. It's a known fact that the
100% of the time, with no exceptions.
pain
1
18
Pain relies on context Part 1
S ensory information, or 'sensory cues', (any information coming from your senses, including your body) needs to be evaluated by your central nervous system. Evaluation of these cues is extremely comprehensive; it involves complex memory, reasoning and emot ional processes, and must include consideration of the potential consequences of a response' 5.
The context of the pain experience is critical. Here is a simple example: exactly the same minor finger injury will cause more pain in a professional violinist than in a professional dancer' 6 because finger damage poses a greater threat to the violinist. The event plays a greater role in the violinist's livelihood and identity.
19
Reflect back to the first image in the book,
Emotional and physical pain are frequently
the one with the large nail piercing the man's
used terms. Although many people tend to
toe. When you step on a nail in the garden, it
separate these pains, the processing in the
mayor may not hurt immediately. The brain
brain of painful tissue injury and anguish is
has to decide whether pain is appropriate.
probably quite similar. Some pain experiences
Other cues which may exist at the time
include a lot of tissue injury or disease, but
include avoiding other nails, the fear of
there will always be varying emotional
serious damage and infection, and the need to
content. In pain experiences such as grief, or
protect others.
rejection from a loved one, where there is a high emotional content, there will still be physical issues such as changes in muscle tension and altered cellular healing. In a situation where a person has had a work injury, say lifting or falling, and his pain state is denied by a supervisor or health professional, there may be very strong emotional and physical components. The emotional and physical components of a pain experience clearly exist in a spectrum. To effectively deal --M.th pain, it is important to identify the sensory cues. We like to call them the cues that help ignite a pain experience, thus the 'ignition cues'.
pain
1
20
Pain relies on context Part 2
T he issues of context, and thus identification of ignition cues, are so ilnportant in the pain experience. Here are some more examples.
Pain in the office is common. It may be worse when the boss is present, depending on your relationship with the boss. Here the environment is a critical cue and there are likely to be many subplots in the environment. The provocative image drawn here is a reminder of the contribution of gender roles, sexism, sense of control, workload and ergonomics in pain experiences.
A pimple is never desirable. But that pimple will feel enormous and get more painful to touch if you are about to go out on an ilnportant date or business meeting.
Pain is dependent on its perceived cause. For example post-mastectomy patients who attribute pain to returning cancer, have more intense and unpleasant pain than those who attribute it to another cause, regardless of what is actually happening in the tissues'.
21 known for many years that the more information that a patient has about a surgical procedure, even knowing that pain after is quite normal, will reduce the amount of pain killers required after surgery.
The amount of pain a person experiences is influenced by who else is around. In pain experiments, males have been shown to have higher pain thresholds if tested by females 19 . Also, when accompanied by their spouse, a patient with a very attentive and caring spouse will have more pain than a patient with an uncaring spouse 20 • Ask yourself why.
And finally, one of the most common pains on the planet is toothache. It too is dependent on context. Does it hurt more because dental work is expensive? All dentists are In another example, subjects (volunteers!) placed their
aware of the patient who makes an
head inside a sham stimulator and were told that a
emergency appointment, yet the
current would be run through their head. Pain
toothache disappears the moment the person enters the dentist's
increased in line with the instructed intensity of stimulation even though no stimulation was given
18
•
surgery. Toothache is a great example of pain making you take
A lack of knowledge and understanding also creates
action. If your pain has gone, your
its own inputs and enhances fear. For example,
brain-J.s probably satisfied that you
unexplained and ongoing pain and deep injuries that
have taken the required action
you can't see, unlike most skin injuries, increase the
before the dentist has even looked
threat of pain. It also works the other way - it has been
in your mouth.
pain
1
22
The phantom in the body The idea of the virtual body
P hantom limb pain is the experience of
Pain after amputation is usually more
pain in a body part that does not exist.
severe if there was pain before amputation22 .
Seventy percent of people who lose a limb
This is a type of pain memory.
experience a phantom limb. It's not all legs and arms either. Phantom breasts,
Phantom limb pain tells us about the
penises and tongues have been
representation or map of the limb (the
reported'g·2' . We believe that all pain
'virtual limb') inside the brain. In fact,
sufferers could benefit from knowing more
many virtual bodies are held within the
about phantom pain.
brain. Our virtual bodies let us know where our actual body is in space. Try
One of the lessons comes from the
closing your eyes and reaching for a cup.
apparent realness of the phantom limb.
You can still do it because your brain uses
It can itch, tingle and hurt. The phantom
the virtual body to know where the real
limb's symptoms worsen when the person
body is. In phantoms, although the leg is
becomes stressed. The symptoms worsen
missing, the virtual leg and the
when someone comes close to where the
relationship of the leg to the rest of the
body part would have been. Some people
body is still represented in the brain.
have reported feeling rings on phantom fingers, old surgery sites, and hands still clenched as though on a motorbike handlebar. Some report phantom legs that 'can't stop walking'.
23
Children can have phantom limbs even if they are born without limbs 23 . What this tells us is that
THE SENSORY MAP IN THE BRAIN Groups of neurones devoted to body parts (the homunculus) are in a thin strip of brain just above your ear
there must be a virtual body in the brain from birth. This virtual body is further constructed, refined and added to as we grow and do new things. Take, for example, learning to kick a ball. The map of the leg would link to areas in your brain that are involved in balance and coordination and the use of particular muscles.
Perhaps the only good side-effect of a minor brain injury is that pre-existing phantom pains may go. Some studies using brain imaging2426 have shown that phantom pain is associated with extensive alterations in the way that the brain is organised.
J
In fact, imaging studies show that marked changes occur in the brain with any chronic pain situation, not just phantom pain27. These alterations result in changes in the virtual body. For example, in the case of phantom leg pain, the )
brain area related to the leg actually 'smudges' so that there is no longer a clearly outlined virtual leg in the brain.
PHARYNX INTESTINE
pain
1 24
Age, gender, culture and pain
The exact effects of age, culture and gender on pain are
boomgate falls evenly on a 10 year old, a 45 year old and a
difficult to study and are not fully understood, although
62 year old they will all say it hurts at about the same
research in the area is developing quicklY.
amount of force. That said, the response to being struck will vary according to age. A baby will scream, a child will
AGE
cry, an adult may react in various ways.
The medical view has often been that older and younger people feel less pain than middle-aged people. This is not true 2S.29 . The pain management skills presented in this book are of equal use for all ages, with adaptation where necessary. GenerallY speaking, if a railway crossing
The prevalence of some pains, such as back pain, varies throughout the lifetime30 • For example, the over 60s have less back pain than the under 60s. This shows again that pain is not necessarilY related to the amount of degeneration in tissues. We begin attributing meaning to pain from a very earlY age . Have you ever noticed that when infants hurt themselves, they often look to their parents before screaming with pain? Parents can 'inform' infants about the meaning of the sensory input they are receiving (health professionals also inform patients about the meaning of sensory inputs). The earlY impact of meaning has been investigated in association with injections: the second injection a child receives usually causes more pain behaviour (e.g. screaming, avoidance) than the first 31 • Also, during immunisation the pain behaviours of a young circumcised boy are more obvious than a non-circumcised bor2.
25 GENDER
CULTURE
Differences in pain experiences might be due to
Initiations are a great example of cultural influences
reproductive organs andJor societal gender roles . For
- they often involve severe injury but are rarely
example, they might follow stereotypes : mother or father
described as painful. Why would pain be a sensible
roles, women wearing high heels, men with beer bellies,
response when the point of the initiation is to enter
women with big breasts, stereotypical job demands, hobbies
manhood? What about the Easter crucifixions
or sports played. These differences in pain are usually
(voluntary) in the Philippines - little or no pain is
caused by different SOCietal roles not different physiology.
reported. Now, why would pain be sensible when the point of the cruciI1xion is to get closer to God?
There is a popular myth that females have a lower pain threshold and tolerance than males, at least until females
Many studies34. 35 report
go through labour, at which time their pain threshold
differences in pain
and tolerance 'magically' rises . It is more likely many
thresholds and
females will report pain more honestly until they have
responses between
experienced labour, at which time they feel 'obliged' to
people in different
be 'tougher'. There is still a tendency to undermedicate
cultures. For example,
female pain patients in comparison to males, which
the level of radiant heat
suggests health professionals may 'psychologise' the
found to be painful to
pain of females more than the pain of males
33
•
)
Mediterranean peoples is merely regarded as
We should also acknowledge that most pain research to
warm to northern
date has been done on male animals by male researchers .
Europeans 36 • Do Mediterranean people have greater
Perhaps our understanding of pain will change when
reason to consider radiant heat to be dangerous?
these conventions of research change. Your pain will never be the same pain as that
experienced by your health professional or anyone else for that matter.
m
Recap
• All pain experiences are a normal response to what your brain thinks is a threat. • The amount of pain you experience does not necessarily relate to the amount of tissue damage.
• The construction of the pain experience of the brain relies on many sensory cues. • Phantom limb pain serves as a reminder of the virtual limb in the brain.
/
29
The alarm system has to have a command centre, obviously the brain. In the same way your most precious possessions would preferably be stored inside an alarmed safe with soft padding, the alarm command centre is put in the safest place the body can find - in the bony safety of the skull (skull bones are our strongest bones) and nestled in a hydraulically-cushioned environment. There are other subcommand centres too. These are also put in reasonably safe places - next to the bony vertebrae. See page 62.
In this picture, a paper cut has damaged some
tissues in the skin and rung a few alarm bells. But it is more complex than this . Alarm bells ringing does not necessarily mean that there will be pain. If you placed your hand over a hot surface the increasing warmth would begin to ring a few bells and a few messages of impending danger will be sent from the skin in your hand. The process whilch may eventually turn these danger messages into pain is far more complex. In this next section we take a look down the microscope at this remarkable alarm system which exists in us all.
pain
2
30
A closer look at alarm signals Sniffing little reporters can set off alarm bells
A ll over your body there are millions of sensors that can be thought of as reporters constantly surveying their area for activity. These sensors sit in the walls and at the end of individual neurones, which have the ability to convey information towards the spinal cord. See page 60 for more on neurones. Sensors can be quite specialised. Some will respond to mechanical forces (M) such as pinch or pressure. Some respond to temperature changes (T), both hot and cold. Others respond to the presence of chemical changes (0), either from outside your body (e.g. nettles, allergens) or
AB well as the sensors being specialised, the neurones in which they sit can be specialised. For example, the electrical impulses in some neurones travel 150 kilometres per hour and in other neurones impulses travel at only one kilometre per hour. Both of these specialisations mean that the information that the neurones give the central nervous system is quite limited. For example, the spinal cord is told 'increased temperature in my area', or 'increased acid level in my area', or 'DANGER! in my area'. The complex sensations that we are aware of, like 'tearing', 'stretching', 'ripping' and 'agonising', are produced by the brain's construction of events, which is based on its evaluation of all the information available to it, not only the danger messages.
from inside your body (chemicals released by cells, or carried in body fluids e.g. lactic acid). When sensors respond to a stimulus, such as acid or a pinch, they open so that positively charged particles from outside the neurone rush into the neurone. This sets up an electrical impulse in the neurone. These sensors, along with the sensors in your eyes (specialised to respond to llight) , ears (specialised to respond to sound waves) and nose (specialised to respond to chemicals) are your first protection against potential harm. Your brain will be warned about the most dangerous stimuli and if one type of sensor fails another may take over.
MEET SOME SENSORS RESPONDING TO INPUTS
31 VITAL SENSOR INFORMATION
4. Sensors are proteins made inside your neurones
under the direction of the DNA - the greatest recipe 1. Most sensors are in your brain. These sensors are
book of all. There are all sorts of recipes in the DNA
specially suited to chemical activation. All sorts of
- including those for many different kinds of sensors.
thoughts can make alarm bells in the brain ring, just as
The specialised sensors made by a particular neurone
nettles and other stimuli can make the alarm bells in
depends on which recipes are 'activated' . Which
the peripheral nerves ring. Let's start with the sensors
recipes are activated within a particular neurone
in the nerves from your skin, muscles and bones.
depends on your individual survival and comfort needs at the time . The sensor mix is normally relatively
2. When you look at neurones under the microscope,
stable but can change quickly. If your brain decides
there isa lot of action at the sensors. We have drawn
that increased sensitivity is best for your survival, the
a mechanical ( M), temperature (T) and chemical ( C)
DNA can increase the manufacture of more sensors
sensor. A mechanical sensor can be opened or shut
which open to stress chemicals such as adrenaline.
by various chemicals. For example, if you go to the dentist and get a 'pain-killing' injection, the
5 . Similarly, the rate at which sensors are made is
chemicals in the injected drug close the sensors so
normally relatively stable but can change quickly.
they can't detect mechanical stimuli. No impulses go
A change in the rate of sensor production increases
to the spinal cord. The brain doesn't learn of the
or decreases the sensitivity of that neurone to a
danger. Other drugs and chemicals can keep the
particular stimulus. If you have perSistent pain, you
sensors open. For example, the sting of a sting ray,
should take hope from this because the rate of sensor
regarded by anyone who has been stung as the most
manufacture can be reduced if the demands for
painful thing they have experienced, works by
production are reduced.
locking sensors open.
3. The life of a sensor is short - they only live for a few days and then they are replaced by fresh sensors. This means that your a...ensitivity is continually changing. Remember this point. If you
,
I'm a mechanical
are a pain sufferer, it may give you fresh hope.
sensor. I don't do
Your current level of sensitivity is not fixed.
acid man!
pain
2 32
A closer look at alarm signals continued
S o, how do sensors and sensor activity relate to pain?
This book is about pain, but we don't actually have 'pain receptors', or 'pain nerves' or 'pain pathways' or 'pain centres'. However, there are some neurones in your tissues that respond to all manner of stimuli, if those stimuli are sufficient to be dangerous to the
tissue. Activation of these special neurones sends a prioritised alarm signal to your spinal cord, which may be sent on towards your brain. Activity of this type in these nerves is called 'nociception', which literally means 'danger reception'. We all have noclception happening nearly all of the time - only sometimes does it end in pain.
Nociception is the most common, but by no means the only precursor of pain. For example, some thoughts can activate
alar~signals
right inside your
brain without nociception occurring anywhere.
Remember, nociception is neither sufficient nor necessary for pain.
33 Various sensors are embedded in the membrane of a neurone. If a sensor is open, ions flow through. Many sensors are designed to open to specific input. M opens to mechanical forces, A opens to acidic or chemical forces, and T opens to
temperature changes. If there are enough open, positive ions flow into the neurone and send a danger message to t:p.e cord.
Jr >(
>(
x
>(
>(
i >(
>(
y.
'f.. >(
NEURONE
>(
pain
2 34
Sending messages A critical number of open sensors will start the response
N eurones are electrically excitable. Every
level of excitement gets close to the critical level
time a sensor opens and positively charged
of excitement, then even small events that only
particles rush in, the neurone becomes a little
open a few sensors may set off the message . So,
more excited. When more sensors open and the
if this neurone was specialised to carry
excitement inside the neurone reaches a
'danger' messages, then just a small stimulus
critical level, a rapid wave of electrical current
like a tiny movement or a change in
travels up the neurone . This is called the
temperature can be enough to make it reach
'spike', the 'impulse', or more technically, the
the critical threshold and may make it hurt
'action potential'. Action potentials are the way
(depending of course on the current sensitivity
that nerves carry messages - an action
conclusions made by the brain).
'-
potential is a single message . Remember, when we are talking about danger On the graph, the horizontal axis is time
reception, the message that is sent along the
and the vertical axis is level of excitement
nerve to your spinal cord only says 'danger '.
(electrical charge or, for the electricians
It does not say 'pain' . Somehow the spinal
amongst you, the potential difference or
cord and brain has to receive and analyse these
voltage across the membrane of the neurone) .
inputs and create meaningful experiences
Note at the start of the graph, how the level of
which mayor may not include pain.
excitement varies, mainly due to the number of sensors that are open. Also note the critical 'all or none' threshold at which an action
potential (message) occurs. When the actual
35
ACTION POTENTIAL (THE MESSAGE)
w I.:J
'« I-I
o >
-
THE :A.LL OR NONE' POINT
I-
Z
w L w
CRITICAL LEVEL OF EXCITEMENT
I-
U
>< w
t
SE~SORS OPENING
MORE SENSORS OPENING
TI M E
pain
2 36
The alarm message meets the spinal cord
INHIBITING CHEMICALS (HAPPY HORMONES)
W
hen the message reaches the end of the
neurone in the spinal cord (inside your back or neck) it causes chemicals to be poured out into the gap (synapse) between the end of the neurone and neighbouring neurones. Many neurones from the tissues converge onto one going up to the brain. Each neurone releases a certain mix of chemicals into the synapse. At the other side of the
TO THE BRAIN
synapse is a neurone that has chemical sensors, specialised to respond to some chemicals but not others. Basically, round
SENSORS EXCITATORY CHEMICALS
chemicals fit in round sensors, square chemicals in square sensors, etc etc. If they fit, they open the sensor. This is called the 'lock and key' principle. You have just completed second year university physiology.
MESSAGES FROM THE TISSUES
37
Some of these sensors in the next neurone act for day to
degree, its activity is controlled by the central post office
day danger messages: some are special memory sensors;
(brain). In fact, the central post office (brain) can even
some are reinforcing sensors and some sensor activity
shut down the regional office (spinal cord) via a very
can be reinforced by activation of the immune system.
powerful internal danger control system.
When your whole body is under threat, for example when you have the flu, increased sensitivity is a
How is that done? A pathway comes down from the
common feature.
brain to meet any arriving impulses. Have no doubt about the strength of this pathway, so powerfully shown
A danger message will pour particular (let's say round)
in the amazing pain stories. In fact it is approximately
chemicals into the synapse. The round chemicals are the
60 times more powerful than any drug you can inject or
keys to unlock the round sensors on the second
ingest. It allows a flood of chemicals (happy hormones)
neurone. When the excitement level of the second
such as opioids and serotonin, which are different in
neurone reaches the critical level - WHAM! - an action
shape and which therefore activate different sensors.
potential - the second neurone sends a message up to
These sensors make positively charged particles leave
the brain. This message says 'Danger!' This is why these
the neurone, which makes it less excited, which in
second neurones are called 'second order nociceptors'.
turn makes it less likely to send a message. So, the
We call them danger messenger neurones .
descending input dampens down the alarm signals.
The synapse is an important sorting site - a bit like a
Yes, with this system, you can win the grand final or
post office. The inputs and outputs of a post office are
the world championships or cook for twenty while still
constantly changing. If there is a party in the post office
carrying injuries .
and everyone is excited, all sorts of messages may pass. However, this is just a regional post office and, to some
pain
2 38
The message is processed throughout the brain Lots of others are processed at the same time
So, the danger messenger nerve takes the danger message
There is not just one pain centre in the brain, as
up the spinal cord into the brain. The danger message
people used to think. There are many. We call these
arrives along with a lot of other messages and they are all
areas 'ignition nodes'.
processed by the brain. The challenge for the brain is to
construct as sensible a story as possible, based on all
These brain parts include clusters of nodes used for
the information that is arriving. The brain 'weighs the
sensation, movement, emotions and memory. Pain just
world' and responds by doing many things, one of which is
borrows these parts to express itself. In chronic pain, some
giving you a perception of what is happening. One way to
of these nodes are hijacked or even enslaved by the pain
)
think of pain is that it is part of the response of the brain
experience. It's almost like an addiction to pain.
to the information that is arriving. In the figure, we have identified the parts of the brain that
In the last ten years, technology has allowed scientists to
are usually active ('ignited') during a pain experience.
take pictures of what is happening in the brain when
These parts all link up to each other electrically and
people experience things such as pain39 .40. We have learnt
chemically. It's a bit like the picture you find in the back of
more about the physiology of pain in the last ten years than in the previous thousand years.
an airline magazine that shows all the routes across the country. The particular pattern of activity which creates the perception of pain can be considered a 'neurotag' for pain.
One of the most important things that we have learnt is that in a pain experience, many parts of the brain are involved simultaneously. Although consistent patterns can be seen during pain experiences, the exact parts and amount of activity vary between people and even between measuring occasions in the same person. Every pain experience is unique.
We acknowledge its origins from Melzack's neuromatrix 79 •
39
Now, we have to acknowledge that the danger message from the tissues via the spinal cord is j ust one of the inputs. Although that message plays an important part in the processing in the brain, especially acute pain, on its own it is not enough to cause pain . Remember the story of phantom limb pain (see page 22). The actual body part doesn't even exist, but it hurts, yet brain imaging studies show activity in all the same brain areas, including the virtual limb.
A POSSIBLE PAIN NEUROTAG I. PREMOTOR / MOTOR CORTEX organise and prepare movements
2. CINGULATE CORTEX concentration , focussing
3. PREFRONTAL CORTEX problem solving , memory
4 . AM YGDALA fear, fear conditioning, addiction
S. SENSORY CORTEX sensory discrimination
6. HYPOTHALAMUS/THALAMUS stress responses, autonomic regulation, motivation
7. CEREBELLUM movement and cognition
8. HIPPOCAMPUS memory, spac ial cogn ition, fear co ndit ioning
9. SPINAL CORD gat ing from the periphery
pain
2 40
The orchestra in the brain
O ne way to think about how the brain works,
And this orchestra is awe-inspiring. It is actually
including how it produces pain, is to think about
a yellowish lump of neurones, the consistency of a
it as an orchestra. A skilled orchestra can play
soft-boiled egg. It contains around one hundred
many thousands of tunes. It can play the same
billion neurones, each of which can make
tunes with clifferent tempos, in different keys, with
thousands of connections. There are more
clifferent emphases, and with clifferent instruments
possible connections in the brain than particles in
taking different roles. New tunes can be made up,
the universe. Neurones are so keen to make
old tunes revived, variations improvised,
connections that a single neurone placed in a
depending on the audience. Pain can be thought
saltwater bath will wriggle up to 30% of its length
of as one tune that is played by the orchestra.
in search of another neurone 4l • Babies make millions of synapses per second, 3 million
A good orchestra can play all the tunes. And can
synapses fit on a pinhead42 ,43. You, the reader,
easily learn more tunes. However, if the orchestra
have a dynamic ever-changing brain; millions of
plays the same tune over and over, it becomes
synapses link and unlink every second. You could
automatic, it goes by memory, it becomes more
donate 10,000 synapses to every man, woman and
and more difficult to play anything else. Curiosity
child on the planet, and still function reasonably!
and creativity becomes lost. Audiences stay away ...
~ I
J
41
! I I
:J ~ I
I
~
~
~
J
~
J ~ ~
J
pain
2 42
Systems to get you out of trouble A tune will always have some effect
M
essages into the brain do not end in the
In a threatening situation, and especially during
brain. In a dynamic living system what goes in
pain, these systems will work really hard for you.
must come out in some form. As part of the brain
They are at their best for short periods. During
weighing the world, it makes a value judgement
pain, the activity of the systems is like a sprinter
on the inputs and responds . When you are cold
who performs at a high level of activity for a short
there are many ways your brain and body can
period. However, if you are in pain for a long
respond. When you are in danger, the brain calls
time , the activity of these systems starts to cause
upon many systems to get you out of trouble.
other problems - they can't be expected to sprint
These systems are working all the time. The most
for a marathon. In section 4, we discuss the
obvious examples are: the muscle system, which
consequences of long-term activation of these
enables you to run away, splint an injured part,
protective systems.
hide or fight, and the sympathetic system, which controls sweating and blood distribution. Other systems such as the immune and endocrine systems work silently but diligently. Together, all of these systems help to create a pain experience, or a motor experience or a stress experience. All these systems can help you get out of trouble.
43 SYMPATHETIC NERVOUS SYSTEM increase heart rate, mobilise energy stores, increase vigilance, sweat
MOTOR SYSTEM
run away, fight, protect damaged area
ENDOCRINE SYSTEM
mobilise energy stores, reduce gut and reproductive activity
PAIN PRODUCTION SYSTEM motivate to escape and seek help, attract attention
IMMUNE SYSTEM
later : fight invaders, sensitise neurones, produce fever, make sleepy to promote healing
PARASYMPATHETIC SYSTEM
later : nourish cells, heal tissue
1
Recap
• All pain experiences are a normal response to what your brain thinks is a threat. • The amount of pain you experience does not necessarily relate to the amount of tissue damage. • The construction of the pain experience of the brain relies on many :;ensory cues. • Phantom limb pain serves as a pEminder of the virtual limb in the brain.
Recap • Danger sensors are scattered all over the body. • When the excitement level within a neurone reaches the critical level , a message is sent towards the spinal cord. • When a danger message reaches the spinal cord it causes release of excitatory chemicals into the synapse. • Sensors in the danger messenger neurone are activated by those excitatory chemicals and when the excitement level of the danger messenger neurone reaches the critical level, a danger message is sent to the brain. • The message is processed throughout the brain and if the brain concludes you are in danger and you need to take action, it will produce pain. • The brain activates several systems that work together to get you out of danger.
47
....J W
> W ....J
z « I:L
INJURY MOMENT
HEALING TIME (DAYS / WEE'KS)
pain
3
48
Acid and inflammation in the tissues
Acm IN THE TISSUES
INFLAMMATION IN THE TISSUES
The alarm system works for you all the time. Frequently it
Anything with '-itis' on the end refers to inflammation:
makes simple calls for change. Take for example when you
tonsillitis - inflammation of the tonsils; tendonitis -
don't move for a while, or you are sitting on a rock which
inflammation of a tendon. Inflammation is designed to hurt
creates pressure on your bottom. Movement is important to
- and it does. Remember your last sprained ankle, or
keep your system flushed . A lack of movement, or a
toothache, or appendicitis. Inflammation is a primitive
physical obstruction, like sitting on a rock, leads to a fluid
form of defence that is essential to the tissue repair
build up in your muscles and joints of the by-products of
process. Think of the swelling, redness and pain after
cell activity - including acid. Have a look at Mr Lee, now in
injury as part of your own internal repair system and be
his pyjamas after a long day. He has been at the computer
grateful for it.
for too long. In such an instance, the acid build-Up in muscles and other soft tissues makes acid sensors open, which leads to impulses running up to your spinal cord and perhaps on to your brain. If your brain concludes that your muscles are in danger (which would seem logical) and you should do something (which also seems logical) then it will hurt . The solution? Move. Just move. Any kind of movement. Random movements are best.
In fact, the thought of 'acid tissues' should make us all get up and move. This is cheap treatment - no drugs are needed, nor fancy therapies.
49
NAI L
PHAGOCYTES &
Here is a close-up view of the nail lodged in the foot. There is
(
Inflammation makes joints stiff in the morning, produces
a lot happening and it is all about repair. Blood vessels may be
sharp pains, redness and warmth. Often, anti-inflammatory
damaged and small nerve endings stretched. Small cells, which
drugs such as ibuprofen, naproxen, aspirin and paracetamol
normally just hang around waiting for trouble, release
reduce the effects including the pain. Anti-inflammatories
histamine, which makes blood vessels release plasma, which in
probably work by stopping the production of prostaglandins 44 ,
turn causes more swelling. This process releases white blood
which are key sensitising chemicals in inflammation. The
cells and delivers cells that mop up the mess in the area and,
swelling, which is the most obvious part of inflammation and
if the skin has been broken, deal harshly with any bacteria
which worries so many people, is just a by-product of the need
(
present. These cells are called phagocytes and macrophages.
to get blood and healing chemicals into the area.
(
Cells that help scabs form and create scar tissue are also activated. Damaged nerves may also release chemicals, see page
Note that we are talking mainly about acute inflammation.
64, that aid the process. This swelling is called 'inflammatory
Chronic inflammation is a part of certain disease states such as
soup'. Inflammatory soup directly activates alarm bells and this
rheumatoid arthritis and can have different and extra effects.
increased sensitivity is designed to protect the injured tissue.
pain
3
50
Inflammation: The brain is immediately interested I nflammation accompanies fNery tissue injury and the brain
With a nail in the foot, the brain will be computing and
will nearly always be interested. Not just in nails in the feet,
retrieving information about previous similar events, trying
but strains and sprains and all sorts of injuries. Humans
to determine the best way to respond. There will be
are able to draw on a wide variety of cues in order to make
computations related to a previous injury. Do I need a
the danger message meaningful. We thought it important to
tetanus shot? When was my last tetanus shot? There will be
remind you of this as you think about injured tissues.
computations about the immediate circumstances. I should move the nail in case someone else stands on it. How silly
Think back to the man with a nail in his foot. Think about
will I look later? I haven't time for this! Is the blood
what other cues might be used by this man's brain in order
making a mess? There will also be computations relating to
to construct the most meaningful response, including the
the future . Is my Fred Astaire dancing career finished? Will
pain response, the motor response, the sympathetic, immune,
I need crutches? Will I have to go to hospital? Will it get
and endocrine responses . After all, this man needs to draw
infected? There will be further computations related to
on every piece of information that will best serve him in
similar events in the lives of others. Will I end up like that
the quest to protect and preserve (Charles Darwin would
woman on the Jerry Springer show? Will I be treated by
argue it is all in aid of making sure that by the time you
that new doctor at the hospital? Or computations related to
die, you have more offspring than the next person) .
livelihood. Can I work? Will I need to get new shoes? Can I get compensation?
The amazing thing is that this man may have no idea that his brain has considered any of this. All he knows is that it hurtsl
51 THE SENSORY CUES FLOOD IN
pain
3
52
The truth about muscles
M
uscles get a lot of blame for pain.
This pain can hang around for a few days
Advertisements for products to manage muscle
and may be quite worrying if sufferers don't
pain abound and it is easy to think that you have
understand why. Delayed muscle pains often
torn a muscle. But let's see if we can put muscle
occur after eccentric exercise where muscles
pain in perspective with these six key pOints .
contract as they lengthen. But in general , muscles are very responsive, stretchy
1. Muscles have many sensors in them so they
can easily be a significant part of a pain
structures. They have to be to protect you and allow you to express yourself.
experience. 4. Muscles have a great b lood supply, so when 2. Muscles can become unhealthy and weak,
they do get injured they are champion healers.
especially if they are underused, or used in
After all, movement and protection are so
ways to which they are not suited.
important to our survival. If you have ever damaged your tongue, you would know how
3. Muscles are actually quite hard to injure. Sure
they bruise a bit, microtears (small injuries to the lining of muscle fibres) can happen, but it is difficult to severely injure a muscle. There can be a build-up of acid, which will make the alarm bells ring, and sometimes new exercises can be associat ed with delayed onset pain in muscles - perhaps eight hours after activity.
quickly it heals. Tongue is made of muscle: eating and speaking are important .
53
s. Altered muscle activity is part of your response to injury and threat. Changes in muscle activity in the short term serve short term purposes - like escape, or bracing, or efficiency45 . But, in the long term there can be costs. We discuss this on page 90.
6. Most muscle activity is about making sense of
the world and how to cope with it. In this way, muscles are windows onto the brain. So if your muscles are working differently you must ask yourself whY. Tone of voice is determined by muscles in your throat . Spasm is a powerful protective muscular process. So are limping and other protective behaviours. It is the brain which allows freedom and quality of muscle expression. Without muscles, you can't walk, talk, laugh, lie, wink, spit, fart or cry.
pain
3
54
Get to know your LAFTs Formerly known as discs
' Disc' is an unfortunate name for the remarkable
Since then, all sorts of therapies have been aimed at the
structures that intermarry vertebrae. They are not, at any
LAFT. Current approaches include: manual techniques of
stage of life, like discs. In anatomy and medical books, they
manipulating it and squeezing it backwards; surgical
are usually drawn in a manner that makes them
techniques of removing it or snipping pieces off; injecting
recognisable as discs, but such drawings bear no
it with extract of pawpaw (papaya); and superheating or
resemblance to the real thing. In drawings, discussion and
burning it. Practitioners of the various techniques have
diagnoses, they are made to resemble free-floating frisbees.
reported some successes, but nothing has been overly
VERTEBRAE
They are not like frisbees! We
successful for back pain. The fact that very different
suggest they should be called
techniques are aimed at the same structure suggests that
'living adaptable force
LAFT injuries are not fully understood.
transducers' (LAFTs). (Which, incidentally, means
LAFT injuries also attract some very strong adjectives like
that between the 5th lumbar
'ruptured', 'crumbling', 'degenerated', 'herniated' and
vertebrae and the pelvis is the
'slipped'. These words alone are strong enough to stop you
'last LAFT').
moving properly and they may not be giving you a true indication of what is happening in the LAFT.
LAFTs are firmly integrated with adjacent vertebrae and
LAFTs have become so famous and blamed for so much that
are made of the same material
people often think about them in isolation. The figure to the
as your ear plus some super
left shows a stylised LAFT. Note that it is attached to the
strong ligament. In 1934 a
surrounding bones and also note the concentric shock
famous study'6 showed that
absorbing rings that give it the look of a squashed onion.
the LAFT could swell onto a
The joints and vertebrae are surrounded by lots of ligament
nerve in the lumbar spine.
and muscle.
55 LAFT facts
1. The outer layers of all LAFTs have a nerve supply47,
4. LAFTs never slip. They age, bulge , sometimes
so danger sensors can be activated if those layers are in
herniate, and sometimes squeeze onto a nerve or
danger. If the LAFT is injured, surrounding structures
release chemicals that irritate a nerve . Despite these
also full of danger sensors are probably affected as well.
dramatic sounding changes this does not necessarily
In fact, the nerve supply to the LAFT is not as rich as
alarm the nervous system.
the nerve supply to surrounding ligaments and bones. Remember that we are in the area of the spinal cord so
5. LAFTs heal slowly, but they will always be a bit tatty
it is sensible to pack the surrounding tissues with
around the edges. Age changes may be indistinguishable
danger sensors - wouldn't you install a sensitive alarm
from injury changes.
system to protect your most precious possessions? 6. LAFTs, spinal jOints and nerves are not delicate
2 . An injured LAFT may not necessarily cause instant
structures. Watch a person playing sport and
pain. A 'slow pain' perhaps 8 to 12 hours after the
contemplate the forces that go through these structures .
injury may occur as the LAFT slowly inflames. Frequently, a LAFT injury will result in pain and stiffness the day after injury.
3. LAFTs degenerate naturally. Degeneration is a
normal part of aging of all tissues . It does not have to contribute to a pain experience. The LAFT is married to the bones (vertebrae) around it and they stick together and age together and dance through life. At least 30% of people who have no low back pain, have LAFTs bulging into their spinal canal, sometimes markedly. This fact has been known for many years but it is still not common knowledge among the general public 48.4 9 •
pain
3
56
Get to know your skin and soft tissues
A dults have nearly 2 square metres of skin. Skin makes
The strange creature pictured at right is a homuncular
up about 15 to 20% of body weight. Skin is only half a
man. Contained in a little strip of brain (sensory cortex),
millimetre thick on the eyelids but could be as thick as six
which is as long as your finger and just above your ear, is
millimetres on the soles of the feet and the back. The skin
the representation of the skin in the brain. This means that
is a critical protector and as the first physical contact with
if you put a pin in your finger, the virtual finger in the
the outside world, it contains many alarm bells.
brain would 'light up' . Al~ skin (all body parts too) has a little section devoted to it in the brain. However, some parts
Much of what we know about pain is based on the skin. In this sense, it mirrors the state of the nervous system. Interestingly, an injury to the skin very rarely leads to chronic pain, with the exception of severe burns. That said, painful skin zones, changes in skin health and altered sweating or hair growth can all be indicators of damaged nerves.
of brain devoted to areas of skin are out of proportion to the body size. For example, the brain areas devoted to the lips, hands and face are larger than the trunk or leg. If it was assembled as it is in the brain then humans would look a little bit like this odd figure . This suggests a use-dependent brain. The areas that you use more and which require the
In some pain states that are initiat ed by j Oint or nerve damage, skin can be sensitive to light touch and brushing. Sometimes, even the touch of an item of clothing may evoke
best sensation have a larger brain representation. If you demand more of a body part, then that part will have a bigger representation in the brain. For example, violinists,
severe pain. Of course, light touch would not normally be
cellists and guitarists have a bigger virtual hand in t he
able to evoke pain unless the skin is badly damaged.
brain than non-musicians 5 0 .
However, if there is a change in the way the nervous system works and the alarm system is altered, gentle touch or small movements may cause pain. The pain that is common aft er shingles (post-herpetic neuralgia) is a good example. We will discuss nerve changes in the next section.
57
Some more skin and soft tissue facts
HOMUNCULAR MAN Size of body port represents area of brain devoted to sensation.
1. Damaged skin heals quickly, much faster than
ligaments and muscles. It is such an important protector, it has to heal fast.
2. Skin has a high density of sensors , including alarm
sensors, for heat, cold, mechanical forces and various chemicals. See page 30 for a review of sensors.
3. Skin is usually very mobile. It slides as we move . It doesn't like to be scarred. It likes movement .
4. Fascia lies under the skin. Fascia is a tough, strong
tissue, also containing a lot of danger sensors. Fascia is connected throughout the body in sheets and sometimes links to muscles.
5. When you massage skin, you are moving tissues
and also sending useful impulses to the brain. So, movement and touch are useful ways to refresh your 'virtual' and actual body.
pain
3 58
Bone and joint contributions to pain
B ones and joints are often blamed for deep, movementrelated pain. This may make people fearful of movement
It's deep in
because they are afraid it will injure their jOints. We
here Doctor! ,
have all grown up with the concept of pain 'deep in the joint' and 'in the bones'. Many a patient has said 'I need to get a bit of oil into my joints'.
There are 206 bones in the body and many more joints. Bones are not normally brittle. They absorb pressures well and will adapt and change their shape in response to the body needs. Bones are living, healing structures. They are full of danger sensors and so are jOints. Bones are covered in a supersensitive layer (the 'periosteum'), which acts as an extra protection system - no-one likes getting kicked in the shins!
Joints come in different shapes and sizes. Some are fibrous with interlocking bones, for example the joints
sensors - especially the synovium, which is the layer of
in your skull. Most are synovial jOints (e.g. hip, elbow,
tissue that makes the lubricating fluid. These danger
finger joints), which means that the joint cavity is
sensors can go berzerk with injury or inflammatory
enclosed and contains a slippery lubricating fluid. The
diseases such as rheumatoid arthritis, which frequently
linings inside these joints are particularly full of danger
result in very painful jOints.
59
Here are some bone and joint facts
1. Joint pains are often described as grinding, stabbing,
4. Joints adore movement and regular compression,
gnawing and aching. However, these words are brain-
which are essential for their health. Movement
derived constructions based on the input from the
distributes the slippery synovial fluid, and cartilage
joint plus a whole lot of other inputs. Part of the
loves the pumping compression. The brain eagerly
reason we describe joints as grinding is because that
welcomes the sensory inputs from the joints as it
makes sense mechanically.
wants to know what is happening so it can construct the best responses for you, (e .g. it tells you to alter
2. An important factor related to joints and pain seems
balance or position) .
to be the speed at which jOints are damaged - if the changes are slow, the brain probably concludes that there is no real danger. The pain of dislocation,
5. Smashed bones can heal, sometimes stronger than
before. The repair process is powerful!
inflammation and fracture is undeniable, but most people with worn jOints never know about it.
6. Some joints in your back or neck can get injured, e.g.
in car accidents, but the injuries can be too small to 3. Our bones and joints are not attractive when x-rayed,
see on x-rays and scans 5l . Your brain may have
especially if we are a bit older. We all have worn joint
recognised the threat, however, and ring alarm bells,
surfaces and little bony outgrowths. X-ray findings
which may, or may not, result in pain. Remember,
do not necessarily match pain. Changes are likely to
though, activity of the alarm system (nociception) is
be age-related changes (the kisses of time) .
neither sufficient nor necessary to cause pain.
pain
3 60
The peripheral nerves Get on your own nerves
M
ost people know about muscles and jOints. You can see
The best way to learn the key facts about nerves is to get on
and touch them. You often see pictures of them on medical
your own nerves . Find the point of your elbow (olecranon)
clinic walls . Unfortunately, nerves are often forgotten.
and then find the bony point a few centimetres away from
There are hundreds of metres of peripheral nerves in your
the olecranon towards your body (medial epicondyle). The
body. The peripheral nerves connect the brain and spinal
ulnar nerve travels right between the two pOints. If you
cord to your tissues and thus to the outside world. This makes them really important, especially if a nerve gets damaged or stops working properly. Leading neuroscientists argue that peripheral nerve problems are far more common than clinicians believe52. 64 •
then go a few centimetres towards your wrist (check Mr Lee) and rub your finger sideways you should roll over the ulnar nerve. Notice that it is at least half as thick as a pencil, and slippery too. There are tens of thousands of transmitting fibres (neurones) in this nerve and they will transmit impulses while you move and stretch. If you run your finger back and forth across the nerve you will probably get some pins and needles in your little finger. You have probably opened a few mechanical sensors and the nerve is reacting normally.
Look at the nerve image. Nerves are cords. They are about 50% ligament, which makes them quite strong, and about 50% neurones . Some of these neurones inform the spinal cord and brain about activity of the sensors and others drive muscles and sweat glands.
61 Helpful things to understand about nerves
I. The ligament part of a nerve has danger sensors
in it just like any ligament in the body.
6. Nerves change appearance with age . They can
become a little thinner or, in areas where they 2. The neurones in a nerve can be a real source of
danger messages and a contributor to pain. This
need more protection or where they rub a bit, e.g. the wrist, they can become thickened.
is due to an increase in the number of sensors at a damage site. Some of these sensors may be
7. All the fancy scans and conduction tests in the
activated by mechanical stimuli, some by lack of
world may not necessarily identify a damaged
blood, and some by stress chemicals. If there are
nerve, but minor nerve problems can be very
enough sensors open the damaged area of nerve
troublesome. They are usually sensitive to
can 'ignite' and send danger messages .
mechanical forces such as pressure or stretch56.
3. If a nerve is injured and your brain computes
8. Sometimes nerves can be injured but not create
(rightly or wrongly) that more sensitivity is
danger messages for days or weeks. This is
required for your survival, more stress sensors
because slightly different alarm systems can be
may be made by the DNA in the neurone and put
activated when nerves are damaged.
into the nerve membrane. This means that various stress states may contribute to nerve sensitivity. 4. Nerves can be injured by cutting, too much
squeezing and pulling, by irritating chemicals around the nerve, and by sustained reduction in blood supply'5.
5. All around the body, nerves slide as you move .
Injury or diseases which alt er this movement may lead to pain when you move 55.5 6 .
SKIN
pain
3
62
The dorsal root ganglion - the peripheral nerve's minibrain T here is a little bulge in the peripheral nerve just where it is about to enter the spinal cord. This bulge is important because it contains the nuclei of the neurones. The bulge is called the dorsal root ganglion (DRG). It is effectively a 'minibrain' because it is the first place that messages cOming in from your tissues can undergo some modulation and evaluation. You could say it is the most peripheral place in which you think! Some interesting features of the DRG 1. All the sensory neurones that make up the peripheral
nerve have their nucleus (control centre) in the DRG. The nucleus is where the DNA of the neurone resides, ready to be activated to start making sensors, which are transported to the rest of the neurone. See page 30. This means that anything that affects the DRG can have profound effects on the whole peripheral nerve, including changes in transmission and manufacture of sensors57 .
Fluids such as blood and 'inflammatory soup' (say, produced by a soft tissue injury nearby) can irritate it 6l • Sometimes, when there are arthritic changes in the joints
2. The DRG is really sensitive and changeable. When nerves
nearby, and you bend your head back, the DRG can be
are injured, neurones sprout in the DRG and can lead to
squeezed by the bones around it. Because the DRG is so
all sorts of 'short circuits,58. The bones which are designed to protect it can sometimes actually interfere with it 59 ,60.
sensitive, this sort of thing can really hurt. No wonder some people with neck pain hold their head forward.
63 3. The DRG is particularly vulnerable to whatever is in
your blood, including adrenaline, and to other chemicals·g62 that gush into the bloodstream when you are stressed. Manufacturing more adrenaline sensors to put in the DRG is one of many ways that the body can increase sensitivity. This is great news for the nervous system trying to protect you by producing pain - but bad news for you because you have to experience it (we will talk more about this later). 4. Occasionally the DRG can be 'set off' - especially if
you sustain an injury in the area. Sometimes when this happens, the DRG can just keep on firing. It's sort of like a car alarm. You can move around but it keeps sending messages. It can be a real pain in the neck. Unfortunately, even super-powerful 'painkilling' drugs don't do a lot, though it will eventually quieten down of its own accord. But wait! ... The DRG can also be squashed without pain - think about this : some bodies (especially older ones) that have been donated to science reveal squashed nerves but there is no record of them ever having had pain when they were alive'g6'. You would think they would have been in absolute agony! The most likely explanation for this is that the compression occurred gradually over time, which meant that the brain must have concluded that there was no danger in the tissues. ADAPTED FROM BEAR ET Al,64
pain
3
64
Backfiring nerves
N eurones backfire. Especially if they are injured
69
•
This is
something that most people (including some health professionals!) don't know, but it helps explain some types of persistent pain. We are all familiar with the image of impulses going up to the spinal cord and brain, but neurones are just like a long trail of dominoes - if you start the transmission, it will keep going in any direction available to it 65 • The only reason that sensory neurones most often send messages up the system is that the impulses normally begin at the bottom end! Backfiring happens a lot in the brain, where it is quite normal and all part of an active brain. When it happens in peripheral neurones , it can have surprising effects. When the impulse travels back down the neurone, it causes the release of chemicals at the end of the neurone, wherever t hat may be.
TROUBLE IN A NERVE SENDS IMPULSES BOTH WAYS
These chemicals help damaged tissues to heal. They do all the
This may not be an issue in the short term (unless some
good stuff outlined on page 49 - encourage blood to the area,
drastic treatment measure occurs for a problem that isn't
promote the release of sensit ising chemicals from cells in the
even at the inflamed site) . However, if the backfiring
area and they even signal mop up enzymes to get going and
perSists, sustained inflammation may result, therefore, t he
clean u p . So, by backfiring, injured neurones can actually
problem can worsen because sustained inflammation makes
cause inflammation in the peripheral tissues (for example,
for boggy, soggy tissues. A less sensitive nervous system can
an injured nerve in the back may cause swelling in the foot) .
lessen the amount of inflammation in your tissues .
65
TO THE TISSUES
~:
SENSORS IN DAMAGED
INFLAMMATORY CHEMICALS
TO THE SPINAL CORD
pain
3
66
What you might notice with nerve pain
I njured nerves can create a wide variety of sensations.
What else might you notice?
Thanks to modern neuroscience, most of these seemingly
• Movement often makes it worse. Nerves are more
odd sensations are no longer a mystery. Many common
comfortable in some positions than in others. When a
syndromes such as tennis elbow, plantar fasciitis, and carpal
nerve is sensitive, you tend to favour postures that avoid
tunnel syndrome are likelY to involve peripheral nerves.
putting mechanical load on the affected nerve, e.g. by raising your shoulder up, bending your spine sideways
Common symptoms associated with peripheral nerve pain
66
:
or poking your head forward . • Stress makes it worse - remember that nerves , especially damaged ones, can become sensitive to the chemicals you
What sort of symptoms could there be?
produce when you are stressed. This can be a bit of a
• Pins and needles
vicious cycle. The brain concludes that you are under
• Sometimes burning pain
threat by virtue of this 'unexplained' pain, which makes
• Pain at night, especially in the hands and feet
you produce stress chemicals, which activate the chemical sensors, which fire danger messages, which tell
Where would the symptoms be? • In 'skin zones' or part of the skin supplied by the damaged nerve • Small, mechanically-sensitive hot spots (may be called a trigger point)
the brain you are under threat, and so on ... • 'Zings' . Without warning, when you move, a quick 'zing' may occur53 . It doesn't necessarily happen every time you move. Such unpredictability can lift the fear factor 66 • • Movement or even just a sustained posture may ignite an injured nerve which keeps ringing like a car alarm. This is probably due to DRG involvement53 but it can be reallY disturbing because it just keeps on ringing.
67
Peripheral nerves can produce some really 'odd' symptoms: • after injury there may actually be no symptoms for days, even weeks, then SHEBANG!63 • itchiness in skin zones 67 • it might just feel plain weird. We have heard patients say things like 'it's strings pulling', or 'it's water running in my skin', 'it's ants on me', or 'it's prickly'.
AB long as you realise that, despite some odd symptoms, you are not going crazy! The nerves aren't dying or decaying, they are just doing the wrong thing and in many cases they are responding to signals from your brain that tell them that increased sensitivity and better warnings are required.
Many people have altered, damaged and compressed
nerves, yet no symptoms. If you have nerve pain, and all the cues (e.g. fear, mechanical forces, anxiety) that exist to keep the nerve sending danger signals are taken away, the nerve may not hurt. However, the nerve will still look like it did when it was sending danger signals.
1
Recap
• All pain experiences are a normai response to what your brain thinks is a threat. • The amount of pain you experience does not necessarily relate to the amount of tissue damage. • The construction of the pain experience of the brain relies on many sensory cues. • Phantom limb pain serves as a reminder of the virtuai limb in the brain.
1m
Recap
• Tissue damage causes inflammation, which directly activates danger sensors and makes neurones more sensitive . • Inflammation in the short term promotes healing. • Tissue healing depends on the blood supply and demands of the tissue involved, but all tissues can heal. • The peripheral nerves themselves and the dorsal root ganglion (DRG) can stimulate danger receptors. Normally, pain initiated by danger messages from the nerves and DRG follows a particular pattern.
2
Recap
• Danger sensors are scattered all over the body. • When the excitement level within a neurone reaches the critical level, a message is sent towards the spinal cord • When a danger message reaches the spinal cord it causes release of excita~0ry chem.cais into the synapse • Sensors in the danger messenger neurone are c.ctivated by those excitatory chem'.cals and when the excitement level of the danger messenger neurone reaches the critical level, a danger message is sent to the brain. • The message is processed throughout the brain and if the brain concludes you are in danger and you need to take action, i.t will prod.lce pain • The brain activates several systems that work together to get you out of danger.
71 Take another look at the graph. Injured tissues have
In these situations, the brain concludes that a threat
reasonably defined healing times . However, healing times
remains and that you need all the protection you can
may vary because of associated disease processes, how the
get. There are many explanations for why this occurs.
tissue is used, and the things that people do in life. Reflect
Many of them involve changes in the way the alarm
on the amazing pain stories and a key point from that
system itself works. We've covered the changes that
section - that damage and healing does not necessarily
occur in the periphery in the last section. Changes
relate to pain. We know that pain perSists in many cases
also happen in the spinal cord and brain.
even though the initial injury has had time to heal.
.....J
W
> W .....J
z «
~
•
INJURY MOMENT
HEALING TIME (DAYS / WEEKS)
pain
4
72
Altered central nervous system alarms - the spinal cord L et's hop into the spinal cord before we move to the
The essential neuroscience68
brain. Remember that sensors in the tissues cause danger
The nervous system is highly adaptable and will accommodate most demands that it is given. So, when impulses from inflamed, scarred, weak or acidic tissues keep arriving at
messages to be sent to the spinal cord, which in turn cause the release of chemicals into the synapse there (pages 36 and 37) . Those chemicals activate chemical sensors on the
the synapse in the dorsal horn, or when neurones from the
next neurone, which open and allow positively charged
brain release excitatory chemicals, the neurone in the spinal cord adapts to meet the demand - that is, to get
particles to rush into that neurone, bringing it closer to firing. Remember too that chemicals released from descending neurones from the brain activate different sensors on the neurone. This reduces the excitement of that neurone, and takes it further away from firing. We are in the dorsal horn of the spinal cord. See the figure to remind yourself where that is located.
better at sending danger messages up to the brain. This adaptation begins within seconds of the demand increasing. In the short term, the danger messenger neurone increases its sensitivity to the incoming excitatory chemicals. This means that things that used to hurt now hurt more. This is called 'hyperalgesia'. It also means that things that didn't hurt before now hurt. This is called 'allodynia'. Hyperalgesia and allodynia just mean increased sensitivity. The sensors then change the way they work so that they stay open longer each time they are opened, which lets more positively charged particles into the danger messenger neurone . Finally, the danger messenger neurone increases its manufacture of sensors for excitatory chemicals, including sensors that 'sleep' until they are needed (this is as though a danger memory is placed in the cells) . All of these things change the sensitivity of the danger messenger
NERVE FROM THE TISSUES
neurone . Your alarm system is really looking out for you.
73 More long-term processes also happen - floods of
In a way, your brain is being tricked. It is operating on
sensitivity-enhancing chemicals can swamp the synapse
faulty information about the condition of your tissues .
and some of the incoming neurones can go sproutingo 9 •
But remember - your body and brain are acting in your
For example, neurones which don't even carry danger
best interests - it's to protect you.
messages sprout in close to the danger messenger neurone so that the chemicals that they release activate
Enhanced sensitivity of the alarm system is nearly always
that neurone . This means that just touching the skin, or
a main feature in persistent pain. Remember that the pain
a slight temperature change , might cause danger
is normal, but the processes behind it are altered.
messages to be sent to the brain.
DANGER REDUCING NEURONES FROM BRAIN • about 200 for one danger messenger neurone • releases inhibitory chemicals into synapse • decreases activity when brain concludes danger exists
DANGER MESSENGER NEURONE • tokes danger messages to brain
EXCITATORY CHEMICALS
• increased sensitivity to excitatory chemicals
• in blood stream and released from neurones
• extra sensors for excitatory chemicals
NEURONES FROM THE TISSUES
DANGER ENHANCING NEURONE FROM BRAIN
• transmit danger message from danger sensors
about 200 of these for one danger messenger neurone releases excitatory chemicals in to synapse increases activity when brain concludes more danger exis ts
pain
4
74
The spinal cord as a magnifier of tissue reality Metaphors may make it clearer
F rom the last few pages , it should be clear that when
Here are some metaphors
there are changes in the spinal cord, the brain may no
that may help you
longer receive accurate information about what is
understand this increase
happening in the tissues . Instead of a nice clear view of
in sensitivity:
the tissues, there is now a 'magnifier' or 'distorter ' in the dorsal horn of the spinal cord. One message into the spinal cord is turned into many messages going up to the brain.
• It is as though an
amplifier on a hi-fi system is turned up.
For many people in perSistent pain, this is a critical issue
• It is a bit like someone has
to understand and well worth repeating. In this sensitised
broken into your tool shed
state, the brain is being fed information that no longer
a few times and you have
reflects the true health and abilities of the tissues at the end
to install a super-duper
of the neurones . Put another way, the brain is being told
alarm system - make it
that there is more danger at the tissues than there
infra-red as well as motion-activated.
actually is . The gain of the system is increased. Brain
responses such as movements, thoughts, autonomic and endocrine responses are now based on faulty information about the health of the tissues at the end of the neurone.
• Perhaps you have got a Ferrari engine installed into your VW beetle - one touch on the throttle will really get you moving. • A computer malfunctions. One key stroke on the keyboard (the tissues) such as a P (in the tissues) creates many P's on the computer screen (spinal cord).
75 • 'The spinal cord has a magnifying glass in it. • Noise which was not bothersome before is now bothersome. Perhaps a certain kind or level of music. • The spinal cord is a bit like the tax office. Let's say you had a 'miscalculation' on your tax return one year. The tax office knows that there is trouble with your accounting. Next time you send in your tax return, all the inspectors scrutinise it carefully and will exaggerate any tiny 'miscalculation' you make. It's not fair! • It's like the dripping tap torture on your forehead. Every little drip just keeps getting more and more magnified. ADAPTED FROM BEAR ET AL.B4
Remember the regional post office? (See page 37). The post office staff are now in a perpetual state of paranoia - sending danger messages off at will; the post office starts to send messages on behalf of other localities; letters are sent free of charge; the regional sorting office is sending itself letters via that post office.
The concept of increased sensitivity is often challenging, but this is what happens in all of us when we are injured. This increased sensitivity should fade once the damaged structures are under control, anclJor you fully understand what is going on.
Is that why the princess feels that pea under all those
pain
4
76
The brain adapts and tries to help Smudging the neurotag
L et's move up to the brain. These changes in the spinal
start to overlap. An associated change then occurs: areas
cord will lead to instant changes in the brain. The same
of repeated use get larger. In fact, the more chronic pain
changes which occur in the spinal cord with persistent
becomes, the more advanced the changes in the brain
pain are also known to occur in pain ignition nodes in the
become 7o • We think both types of change are probably
eg 27 . .
brain
Not only does the brain have to process and adapt
strategies by which the brain 'looks out' for you - by
to all the information about the threat, it may change itself.
making the body part difficult to use (smudging of motor
Don't panic, our brains are changing all the time, this is a
areas in the brain), or by making nearby body parts
change aimed at lifting sensitivity, in order to protect us.
sensitive too (smudging of sensory areas in the brain) .
The main changes that occur in the brain are the
But don't panic - reflect on the homunculus again (pages
manufacture of more sensors in the pain ignition nodes
56 and 57) - it is always changing anyway. So if you kept
and of more chemicals in the body to activate the sensors.
stroking an index finger, the area of the brain devoted to
This means it is easier to ignite, for example, a memory
sensing the index finger would start to enlarge. In this way,
area. If you had a nasty accident on a street corner, every
the brain reflects the history of inputs. Braille users have
time you pass that area you may have a reminder, perhaps
larger virtual index fingers71, musicians with painful
just a shudder, or maybe even a pain neurotag is
non-functional hands may have distortion of the virtual
constructed in your brain. Your brain is looking out for
hand in the brain72.
you. Hopefully you are starting to see how sophisticated this protective mechanism can become.
Smudging sounds serious. It probably does reflect changes that are part of a more advanced chronic pain experience.
Another change which is known to occur in the outer
The good news is that it is reversible. In the same way that
brain, the cortex, is 'smudging' - brain areas normally
muscles and joints can be made more healthy and robust,
devoted to different body parts or different functions,
so too can the homuncular arrangements in your brain.
77
SMUDGING IN THE VIRTUAL HAND
pain
4 78
The orchestra plays the pain tune
Orchestral changes We can use the metaphor of the brain as an orchestra to
It is important to emphasise here that, when the brain is
make sense of the brain changes that we've been talking
sensitised, it is not just the experience of pain that is
about, i.e. those brain changes that occur as pain becomes
persistently produced. It also leads to persistent changes in
chronic. It is like the orchestra in your brain has been
sympathetic and parasympathetic nervous systems,
playing the same pain tune over and over and over and
endocrine, immune and motor systems. These systems can
over .. . It can no longer playa full repertoire of tunes . Nor
combine to perpetuate the pain tune, which we call a
can it be creative, curious or seek new musical challenges.
'neurotag', the constant activation of pain ignition nodes .
Key musicians quit because they have nothing to play.
Changes in these systems are discussed later in this section.
Other musicians get tired and sick because they play all the time. Some musicians take over others' roles (e.g. the trumpeters take over the violinist's part). The pain tune is not a happy tune. Tours get cancelled as the orchestra stays home. Audiences stop coming. Record sales drop. You get the picture: the pain starts to dominate every aspect of life work, friendships, family life, hobbies, thoughts, sports, emotions, devotions and beliefs.
79
THE PAIN TUNE
pain
4
80
Thoughts and beliefs are nerve impulses too 'Thought viruses' are very common
T he brain is responsible for making the final decision as
Even thoughts like 'this doctor thinks I am putting it on',
to whether something is dangerous for body tissue and
'the CT-scan couldn't find it so it must be really bad and
action is required. We wrote earlier that, as humans, we
deep', and
have a terrific advantage over non-humans because we can
wheelchair' are threatening to a brain concerned about
plan for events , we can learn quickly from experience and
your survival. These thoughts and the fear of certain
use logic to predict the future . This means that we can
activities, or a fear of re-injury, can increase pain.
~unt
Deidre had back pain and she is now in a
identify a situation as potentially dangerous before there is any input at a tissue level. This is all very well, but when
Thoughts are nerve impulses
the system is really sensitive (as it is in chronic pain),
Through SCientific research, we are now aware of the
inputs unrelated to tissue damage , but judged by our brain
thought processes which are powerful enough to maintain
as dangerous , can be enough to cause pain. This can
a pain stateeg.73.74. We call them 'thought viruses' . Some of the
happen without you ever being aware of it!
most powerful thought viruses known to cause and enhance a low back pain experience (and probably pain experiences
It is well known that some people with persistent pain need only think of a movement or watch someone else perform a movement for it to produce pain. In fact, in some patients, just imagining movement can also cause swelling in the painful parteg l05 . Many patients have told us that 'it hurts if I think about it'. This is completely understandable. You are not crazy. In fact, this is very sensible if you remember that your brain has learned to be very good at protecting you from anything that might be dangerous to your tissues .
anywhere in the body) are described in the figure.
81 All of these thought viruses are common in people with perSistent pain who don't understand the physiology of pain. They are often enough to take you right 'to the edge'.
I'm in pain so there must be something harmful happening to my body.
We can put a man on the moon, why can't someone just fix this pain for me?
I'm staying home, not going out, I'm keeping quiet and out of things.
I'm so frightened of my pain and of injuring my bock again that I'm not doing anything!
Even their whiz-bong scanning machine can't find it - it must be bod.
I'm not doing anything until all the pain goes.
,
pain
4
82
The sensitised central alarm system
S ensitisation of the brain and spinal cord is called central
The pain persists
sensitisation. Read through the common features below.
Self-analysis is needed here. The known healing time for
Perhaps you have some of them. They may provide a clue
tissues involved has long passed. Is there any reason that
that your pain is more related to central nervous system
the damaged tissue wouldn't have healed?
processes than tissue processes.
The pain is spreading Your label
There are no fences in the nervous system. Sensitisation of
Because tissues heal, and because your alarm system and
the alarm system and brain means the brain is (wrongly)
brain have changed to protect you, diagnoses based on tissue
told that more of the body is in danger and the brain
processes no longer fit. Often you end up with multiple
therefore makes more of your virtual body hurt.
diagnoses including fibromyalgia, somatoform pain disorder, chronic fatigue syndrome, myofascial syndrome, non-specific
The pain is worsening
back pain, psychosomatic pain syndrome, repetitive strain
This is the most obvious strategy for your alarm system and
injury, non-specific neuropathic pain. Your diagnosis often
brain if it wants you to escape. Most of the changes in the
depends on where you live and which particular health
alarm system aim to increase the frequency of danger
professional you see. Some diagnoses may have been given
messages sent to your brain. It is, therefore, sensible for
to get you out of the clinic as quickly as possible. The signs
your brain to conclude that the danger level has actually
and symptoms of all of these 'diagnoses' can readily be
increased. This will make it hurt more.
explained by sensitisation of the central alarm system and by contemplating how the orchestra in your brain is playing.
Lots of movements (even small ones) hurt Each increase in the sensitivity of the alarm system will
Because tissues are no longer the main issue, it is often not
reduce the amount of movement that can occur before the
helpful to seek an understanding of the diagnostic label. It
alarm system stops you from going further. If there is
is better to seek an understanding of the particular
ongoing inflammation in the tissues, the danger sensors in
symptoms which are a feature of your unique presentation.
the tissues are also sensitive, further reducing the amount
83 of movement you can perform without pain. When the
Can you identify with any of these commonly
orchestra gets really used to playing the pain tune, even
heard statements:
imagining a movement can produce pain'Sl06. This is a
'It comes on when I think about it.'
highly protective mechanism.
'Watching someone move makes it hurt. ' 'It started off so simply and now it has spread.'
Pain can be unpredictable
'It's worse on Monday. ,
It may hurt one day but not the next. You may be able to
'Now there is
play with your children for an hour one day but not even
'The pain has a mind
pick them up on the next day. Sudden stabs of pain can
'I get lots
a 'mirror' pain on the other side of my body.' of its own.'
of different diagnoses - you nome it,
I've hod it. '
occur which are seemingly unrelated to anything. The
'It gets better with a gin and tonic or a vodka.'
best explanation for this unpredictability is that pain is
'It fol/olNS a seasonal, monthly, weekly or other cycle.'
evoked by much more than the demands on your tissues.
'Treatment only ever gives me temporary relief' 'My pain is worse when I am anxious or depressed. '
There may be a latent period before pain comes on after
'It's the some pain my mother hod. '
an activity. There could be a delay of hours or even days.
'The pain moves around my body. ,
This latency does not usually occur with damaged tissues
'No-one seems to believe me.'
and is a feature of a sensitised central alarm system. With this pattern it is likely that the processes
There are other threats in life: previous, current
underpinning the pain experience are not predominantly
and anticipated
in the tissues, they are more in the nervous system and
Sometimes it is possible to identify physically and
brain in a very real, understandable, and manageable way.
emotionally traumatic events, even from many years ago, that might make the brain more vigilant to threat.
DIAGNOSIS
WHAT THE WORDS ACTUALLY MEAN
Of course, recurrent or multiple traumatic events would
Fibromyalgia
Pain in the muscles and ligaments
give the brain more reason to be protective of the body. Remember, the best way to protect the body is to make it hurt.
S,?ma!of'?r:.m pain disorder
Pain due to neurosis
Chronic fatigue syndrome
Alwals t:::, ir.::: ed'--_ _ _ _ _ __
M yofas.s:~al syndrome
Pain in the muscles and fascia
Non-~ec ific low ba...:.ckc:...c.p=:ai.:..:. n _ _ _ Low back pain not caused by anything in..,p?rticular
Psychosomatic pain syndrome
Pain caused by thoughts and emotions
Repetitive strain injury
Pain started by repetitive movements
Non-..specific neuropathic pain
Pain caused by faulty nerves
pain
4 84
Response systems - the sympathetic and parasympathetic nervous systems The buzz on adrenaline
A
powerful and rapidly responding system that allows you
And remember, threatening cues can come from cuts, cats,
to cope and helps protect you from threat is the
teachers, preachers, leeches, lergies, bumps, bruises, mOvies,
sympathetic nervous system. This is the system which
monsters and muggers (just to name a few).
liberates adrenaline into your body. Normally, adrenaline does a lot of housekeeping in your body for you, for
Together with cortisol (see next pages)
example it regulates breathing and the digestive system.
adrenaline diverts energy to the brain,
It regulates many things that you may never know about,
such as blood pressure.
muscles and heart, makes oxygen available, stands your hair on end, dilates your pupils, constricts your gut,
There are two systems that combine to liberate adrenaline. When required, the inside of the adrenal glands quickly pours adrenaline into the blood. The sympathetic nervous
suppresses immune activity and turns down sperm production76 •76 . All of this is extremely useful as you decide whether to fight or fly (escape).
system - a highly developed network of neurones spread right throughout the body and acting more as a gland than as an electrical system - will distribute adrenaline into all
Adrenaline and pain
The sympathetic nervous system is designed as an on/off
your tissues. With these two systems, adrenaline has
system - quickly activated and then returning to normal
widespread and important effects. It's all brain driven and
(up to an hour later) once the stressful situation has gone.
occurs in response to sensory inputs from the tissues, the eyes and ears, thoughts, beliefs, perceptions, moods and
Chronic pain and stress are usually associated with
memories. The blush that comes to your face if you recall
perSistently increased levels of adrenaline (although
something you might have done years ago, is an example of
sometimes adrenaline can become depleted). Many a
the sympathetic nervous system responding to a memory.
patient has said 'I can't turn the adrenaline switch off'.
85 Adrenaline doesn't usually cause pain by
and this may contribute to the ill health
itself, but with a little help from changes in
and sensitivity of tissues. Not enough sleep,
body parts and heightened alarm system
not enough ongoing repair. This may be a
sensitivity, pain can occur53 • Chronic
good reason to try some relaxation or
inflammation, nerve damage and increased
meditation during the day to try to give the
numbers of adrenaline sensors all mean
parasympathetic system a chance to assist
that adrenaline can magnify the danger
in tissue replenishment and growth.
message and cause pain. Normally, adrenaline is good stuff. The buzz is great, the anger, anxiety and sweating it promotes may be helpful, but don't let it hang around too long.
The parasympathetic nervous system Whereas stimulation of the sympathetic system gives rise to a liberation of energy, the parasympathetic is usually more concerned with slowing and conserving energy - it helps digestion, storing of energy, cellular replenishment, and reproduction. Instead of 'fight and flight', it's 'rest and digest' .
Feeling supported and appreciated are likely to shift sympathetically excited people towards the more protective calming parasympathetic state. The parasympathetic system is more active during rest . Sleeplessness is common in persistent pain
THE SYMPATHETIC NERVOUS SYSTEM AND THE SYSTEMS IT AFFECTS
pain
4
86
The endocrine response
A.ong with the sympathetic and immune systems, the endocrine system is the other key player in the stress response. It works with the sympathetic system but its effects may last weeks or months rather than minutes or hours.
The key bits of anatomy are the stress control areas of the brain (pituitary and the hypothalamus) and the adrenal glands, which perch atop your kidneys. You will be able to see them in the figure.
I ACTH I Threatening inputs, memories and circumstances
back to the brain
make the hypothalamus release hormones, which in turn make the pituitary gland release to all tissues
hormones (adrenocorticotropic hormone or ACTH) into the blood. Within a couple of minutes, ACTH is picked up by chemical sensors
ICORTISOL I
(remember them?) in the outer layer of the adrenal gland. This gland then produces a number of hormones necessary for maintaining a balance in life. A key hormone is called cortisol.
DNEY
87
What does cortisol do? The term 'stress chemical ' is often applied to
Persistent altered levels of cortisol can create a
cortisol, and it sometimes gets a bad rap. But
few problems, though. Increased cortisol has been
remember it is above all a protector. Along with
linked to slow healing, loss of memory,
adrenaline, cortisol is a chemical that protects
depression, despair and a decline in physical
you when you are challenged. It slows down body
performance75. 77.
processes which are not needed for immediate protection and enhances those which are.
Cortisol production changes during the day. It peaks in the early morning, then declines till
So if you have just lifted a very heavy, awkward
lunch when it rises a little bit and then it is at its
weight and hurt your back, or you are in an
lowest in the early evening. Our sensory abilities
armed robbery, or you are about to do a
parallel this. People with maint ained
mathematics exam, you probably have no interest
inflammation often have more pain in the evening
in reproduction and digestion. And any healing of
when cortisol levels are down.
tissues can be put on hold - the processes in inflammation draw too much energy. However, the systems you will need are muscles (to support, run away), and your brain (for quick thinking) and maybe some endorphin support (a brainproduced danger message suppressor). Whether the threat involves a physical or mental challenge, the emergency increases cortisol production.
pain
4
88
The immune system
The immune system is a powerful system that also looks after you, especially when things get bad. It's a key player in pain too, although this is quite a recent discovery. It has close links with the cortisol and adrenaline based systems.
IACTH I
There are immune molecules called cytokines, which are a kind of mobile protective system floating inside the
to the b r o i n
body. Some cytokines promote inflammation and some try to stop it. When you have the flu there will be more of the pro-inflammatory cytokines around. If you
to the b ro i n
ADRENAL GLAND
remember your last flu attack, you may recall that as well as fever and lethargy, loss of appetite etc, your movements were a bit more sensitive and occasionally, old pains may have come back to revisit. This is due in part to the pro-inflammatory cytokines .
ICORTISOL I to the tis 5 U e 5
The brain and the immune system talk to each other all the time and keep up a lively chat with the endocrine, sympathetic and parasympathetic systems. For example, cortisol activates the immune system, the immune system can be stimulated by the sympathetic system, the immune system can signal the brain, the brain activates the cortisol system etc etc.
IMMUNE ORGAN e.g. bone morrow, T-cells
89 Here are some interesting things, relevant to pain, about
Here is a very general list of things that buffer the
the immune system:
immune system75 •82 :
1. The immune system is less involved in everyday
• To have an influence on the quality of one's life
stress and pain. It is more involved when things get serious or chronic.
• To be in control of your life and your treatment options • To have family and medical support
2. Immune system responses can be learnt responses 78 .
• To have strong belief systems • To have and use a sense of humour
3. Long-term stress and pain usually leads to an
alteration in activity which results in more circulating pro-inflammatory cytokines 79 • 4. Immune stressors can be one major event or many
• To exercise appropriately While these behaviours buffer the immune system, they are also known factors to improve a pain state.
minor events (microstressors). 5. The immune system may actually underpin some
pain states, such as 'mirror pain', and loss of fine sensibility. Damaged peripheral nerves are particularly reactive to pro-inflammatory
What is the complete opposite of a stress response?
cytokines80 •81 . A hearty laugh in 6. Finally, the immune system, like other systems, can
be activated not only by events happening in the tissues but by the brain's interpretation of events.
The immune boosting behaviours This is a good time to talk about the immune boosting behaviours, behaviours that you can use to counteract the processes that can combine to cause pain.
a safe place with friends.
,
pain
4 90
Movement strategies
Wehave learnt that the brain produces pain to motivate you to escape. The brain also 'primes' muscles to help you do this. This is great in the short term - you get ready to run away or fight by 'priming' your big long muscles . These muscles are best suited to this job because they can produce a great deal of torque (torque is the twisting force that makes joints move), partly because they cross more than one joint and partly because they can shorten a great deal.
In the long term, activation of these muscles is not smart because they are not designed to be under constant readiness . AB a general rule, when these muscles stay active for a long time, they tend to contract and shorten - then they start to feel 'stiff': there is a build up of acid (see page 48), shoulders get achy, back pain travels up your spine, neck pain spreads to the back of your head or across to your eyes.
91
Alterations in muscle activity may be particularly
These changes may place different body tissues at
important in association with spinal pain. For
risk of injury, or prevent body parts from healing
example, back pain causes changes in trunk
normally.
muscle activity'3. The changes probably help the brain splint the trunk. However, muscle activity
Long-term motor changes make you behave
sometimes doesn't return to normal even if the
differently, hold yourself differently, move
pain eventually resolves
84
•
This failure to return
differently and even talk differently - all of which
to normal is likely to be associated with some cost
have long-term consequences. Once new motor
- the structures of the spine may be more
patterns have been learnt, they can be very hard
compressed, or less controlled. Fear or
to reverse. It's not difficult to pick someone with
anticipation of pain may be enough to prevent
an old arm injury by the way he/she hangs out
changes returning to normal
85
-
it seems that the
thought viruses have an effect on all systems.
the washing, or people with old ankle injuries by the way they walk up stairs.
Recap • All pain experiences are a normal response to what your brain thinks is a threat. • The amount of pain you experience does not necessarily relate to the amount of tissue damage. • The construction of the pain experience of the brain relies on many sensory cues. • Phantom limb pain serves as a reminder of the virtual limb in the brain.
3
Recap
• Tissue damage causes inflammation, which directly activates danger sensors and makes neurones more sensitive. • Inflammation in the short term promotes healing. • Tissue healing depends on the blood supply and demands of the tissue involved, but all tissues can heal. • The peripheral nerves themselves and the dorsal root ganglion (DRG) can stimulate danger receptors. Normally, pain initiated by danger messages from the nerves and DRG follows a particular pattern.
2
Recap
• Danger sensors are scattered allover the body • When the excitement level within a neurone reaches the critical level, a message is sent towards the spinal cord. • When a danger message reaches the spinal cord it causes release of excitatory chemicals into the synapse. • Sensors in the danger messenger neurone are activated by those excitatory chemicals and when the excitement level of the danger messenger neurone reaches the critical level, a danger message is sent to the brain. • The message is processed throughout the brain and if the brain concludes you are in danger and
Recap • When pain perSists, the danger alarm system becomes more sensitive. • The danger messenger neurone becomes more excitable and manufactures more sensors for excitatory chemicals. • The brain starts activating neurones that release excitatory chemicals at the dorsal horn of the spinal cord. • Response systems become more involved and start contributing to the problem. • Thoughts and beliefs become more involved and start contributing to the problem. • The brain adapts to become better at producing the neurotag for pain (the 'pain tune') .
you need to take action, it will produce pain. • Danger sensors in the tissues contribute less and • The brain activates several systems that work together to get you out of danger.
less to the danger message arriving at the brain.
explain
pain
5 94
Introduction Modern management models There are many people and groups of people who would like to help you with your pain. But be careful. A clinical nightmare may be waiting. The more orthodox groups include doctors, surgeons, psychologists and physiotherapists. Slightly less orthodox include chiropractors and osteopaths, and the non-orthodox groups include faith healers and iridologists. Within each group of health professional, there are factions. For example, one surgeon may fuse your vertebrae together (orthopaedic surgeon) while another may insert a stimulator on your spinal cord (neurosurgeon). So too, there are different kinds of physiotherapists, chiropractors, osteopaths, psychologists etc. There is often argument between and within groups.
We are not recommending for or against particular practitioners but suggest that the follOwing guidelines may help: 1. Make sure that any injury or disease which requires
urgent medical attention is dealt with. All ongoing pain states require a medical examination. 2. Make sure that any prescribed help makes sense to you
and to your understanding of the problem. Ask the therapist if there are any scientific studies supporting what is proposed. 3. Have ALL your questions answered satisfactorily.
4. Avoid total dependence on any practitioner. You must take control.
You need to be careful and in control. In particular, be wary because you are likely to hear or have heard many different explanations for your problem. This can make it worse 8 5 and add confusion to your problems. Remember that you are the owner of your pain, more than anyone else. In the end, it is you who has the most power to manage and rid yourself of it.
5. Always have goals that are understood by both you and
your clinician. These could be physical, social and work goals which allow some quantifiable way of measuring progress. Good clinicians have numerous qualities. They are compassionate, enthusiastic and informed. They are
The skills of the practitioners in the various groups may help you with parts of the pain problem, but we believe that you will be better informed and in control if you understand the science behind your pain state.
curious about new ideas. They are experts.
They assist you in mastering your situation.
• • • • • • • • • • • • • • • • • • • • • • • •
95
THE NIGHTMARE OF CHOICE
pain
5
96
Models of engagement Part 1 Think like your therapist
A
ll health professionals have models or frameworks on
which they base their work. You, the person in pain,
J
should also understand these models . We will discuss five current models, which are often used interchangeably. These models should enable you and any clinician with whom you are involved to identify the processes that underpin your pain. We believe that these models should enable identification of any cue that contributes to, ignites, or maintains your pain. 1. The orchestra model
(distributed processing, virtual body, neurotag model) This is the major model on which this book is based. It
acknowledges that even though the processes are
draws from across many pain science disciplines including
happening in the brain, they manifest themselves in very
brain imaging and cellular biology. It considers that pain
real, anatomical and biological ways. Thoughts, ideas, fears
results from a combination of processes in tissues and the
and emotions are seen as nerve impulses which have
processing of danger messages . This processing is carried
electrochemical consequences in the brain, just as inputs
out in many parts of the brain.
from damaged tissues have electrochemical consequences.
The model allows recognition that various ignition cues
If you suffer from pain then strategies that 'run the
(e.g. fear, memories, damaged tissues, circumstances) can
representation' or 'activate the virtual body' without
be a part of the pain experience. It is a model that provides
creating a pain neurotag are required. Put another way, this
an understanding of the biological bases of pain and
means 'to play the orchestra without playing the pain tune' .
•
97 2. The 'onion skin' models The onion skin models adapted from various sources·
d. Pain escape behaviours. For various reasons she g 87
,106
may go doctor or therapist 'shopping', looking for an
help to identify all the factors that contribute to a pain
answer. She may pray, go to lawyers, turn to
experience at anyone time, Pain experiences usually
'recreational' drugs, sleep, travel long distances to
involve inputs from all layers of the onion.
famous gurus, or spend inordinately large amounts of money to find a cure.
Let's use the model to think about the example of a person, say a woman who has had a whiplash injury and still has neck pain and headache a year later (quite a common feature post whiplash):
a. Nociception. Her alarm system is firing from
e. Social environment. Perhaps her family are tired of hearing her complaints and are becoming less and less helpful. She IIlBiY join a whiplash support group and actively chase compensation. She IIlBiY feel that some of her friends do not want to spend time with her anymore.
sensitive, unfit and perhaps scarred tissues in her neck. As we know, firing of the alarm system does not have to hurt but it can be a part of the pain experience. Remember - nociception is neither sufficient nor necessary for pain.
b. Attitudes and beliefs. She feels she should 'soldier on' no matter what and hopefully it will go away, but she realises that this isn't helping. She constantly recalls the accident and has begun to have thoughts that it was her fault and that she might have been driving badly. Common beliefs might relate to the cause of the pain, e.g. 'something is broken in my neck' or 'my pain is punishment for driving erratically'. Beliefs can also foster fear, anger, blame (including 'why me?'), all of which are common in whiplash patients88 •
c. Suffering. At the moment she is suffering in silence, but she feels the need to scream and tell everyone. She is also thinking there is no end to this pain and treatment.
All these things influence, and are influenced, by pain.
pain
5 98
Models of engagement Part 2
3. Fear-based models
In a way, these changes directly promote survival of the
Fear of pain, and fear of re-injuring tissues are extremely
species. Another way to think about it is to reflect and
powerful forces behind the development and maintenance
consider what primitive cave dwelling humans would have
of chronic pain. Models have been developed to use and
done to protect themselves . Just as we have discussed
understand how fear has such a powerful effect on our
inflammation as a protective process not to be feared, so
movements and pain experiences·
g ag
•
too pain is protective.
There are many kinds of fear. Fear is so important in how
5. A clinical decision-making model
you move, behave, feel and think, that we have devoted
Pain is a very personal event. No-one knows the exact mix
pages especially to it (see page 100).
of biological processes that are in action in any particular pain situation, although these days we can make sensible
4. An evolutionary model
hypotheses. If you have chosen a person to help with your
Evolutionists might argue that the object of life is to die
management, we hope that person is an informed clinical
with more offspring than the next species. If we applied
decision maker.
this way of thinking to pain management, then it is easy to see that everything that changes in the physiology of the nervous system is geared up to protect your tissues (this is an obvious theme of the book).
99
Clinical decision making is a vital science in pain management. Your pain is so unique that a 'recipe' for management that is the same for all pain situations will not do. Clinical decision makers should be able to make decisions based on your particular presentation and on the very best of science90 • Ideally, health professionals should be able to give you an answer to all the following questions:
What is happening in my body? How long will it toke to get better? What are all the options for management? What con I do for it? What con you do for it? Is there anything nasty which needs speCial attention? What do my physicol findings, x-rays and scons really mean?
pain
5 100
Fears associated with movement and pain A road map to recovery
Fear is a powerful motivator. It contributes to how you move,
I have a fear of:
o
Pain
behave, and experience pain. The sources of fear are diverse . Fear
o o o o o o
The seriousness of the cause of pain
may be strongly dependent on context, be obvious or be hidden. We have listed some fears that are common in people with perSistent pain. You may recognise some of them.
Not knoWing Not being believed Not being compensated Needing help Certain movements; any movement
O Re-injuring or making it worse
All sorts of fears can lead you into a cycle of pain and disability from which it can be difficult to break free . Some of the information that you receive from health professionals, friends, family and the media may contribute to fear. Of the fears listed, different fears will be relevant to different people in pain at different times. However, all of them can be considered under the same banner that we have mentioned repeatedly: your livelihood as a human is under threat. Remember, in perSistent pain, when the alarm system and brain are sensitised, all of these fears can help maintain the pain by activating those pain ignition nodes - and set the orchestra up to play the pain tune. Remember that the brain wants to protect you from anything that is dangerous . To face these fears, you need to be informed and understand as much as possible about your body. And you will need to be brave - this is the vehicle for the road to recovery.
o Slowing the healing o Not being able to work
o o o o o
Having no income, or money
o o o o
Having sex
o o o o
Not playing With the kids Not looking after the kids/parents Not being able to have kids Not being able to keep the house clean The garden turning into a jungle Not playing sport Cracking (spinal manipulation) Cracking up (nervous breakdown) Getting old Looking bad; becoming overweight Ending up in a wheelchair
o
Driving; not being able to drive
o
What others think; losing friends
o Getting divorced; staying single o Therapy; needles; surgery; botched surgery o Drug addiction
101
11'111:.);1
•
UNDERSTANDING CONFRONTATION
•
,
, ,, , I
I I
.......
_---
~ormation . treatment therapist/patient interaction L--
patient attr_ib_u_t_ es_ _---'
lBi.6i.Q:wHERl]
' ... -- '' ,
I
•
AVOIDANCE CITY
• I
'1%1;1+4'1
ADAPTED FROM VLAEYEN AND CROMBEZ89
pain
5
102
(
)
Coping with life and pain It's a wonder we don't all have chronic pain
It'S not all fear. We face numerous everyday coping issues.
Active coping strategy examples
Coping is the ability to identilY, manage and overcome the
• Learning about the problem
I
issues which stress us all. We all have varying coping
• Exploring ways to move
[
strengths and weaknesses but we can all enhance our ability
• Exploring and nudging the edges of pain
to cope. We use the same body systems to protect us from
• Staying positive
psychological and physical threat.
• Making plans
A more accurate way of understanding this is to
Passive coping strategy examples
acknowledge that all threats to coping involve physical and
• Avoiding activity
psychological processes (the mind and body).
• Doing nothing • Waiting for something to happen
We cope in various ways - emotionally via strategies designed to limit emotional disruption, or by problem solving (perhaps via seeking education, understanding and changing thoughts and beliefs). Coping aims to reduce the
threat value of the stimulus and the associated emotions and altered biology 91. We have written this book in the hope that it will help in this way too .
Consider also the passive and active strategies that people employ in order to try to cope. Active copers manage pain and many other health issues better than passive copers 92 •93 •
• Believing someone else has the answer
,
103
pain
5 104
Your relationship with pain How are you travelling?
B efore we talk about the most important management
Graph 2 is the 'boom-bust' pattern. Pain comes on but you
tools, we believe it is important for you to get an idea of
persevere, you tolerate it as much as you can, and try to
how you are 'travelling' - for you to understand the
ignore it, keep going, distracting yourself ('boom') until
relationship between your pain and your activity level. This
suddenly your pain is unbearable and you 'bust' - flooding
will not only further demystify your pain but will allow you
your nervous system with danger chemicals and leaving
to establish a starting point, a baseline by which you can
yourself completely wiped out for days, maybe even weeks.
evaluate your progress. You can do this yourself, although
In our experience, this pattern is more common in people
you may benefit from a helpful, thinking, informed, clinical decision-making professional.
who are perfectionists, high achievers, energetic, or who perceive that other people or institutions are in control of their situation.
Do you recognise either of the following activity relationships with pain? Graph 1 is the gradual decline pattern. Pain kicks in at a
certain amount of activity, for example cycling, walking a certain distance, using a computer for a certain time, or attending a lengthy function . The natural response is to stop the activity when pain starts. Over time the amount of activity at which pain is experienced slowly reduces, eventually leading to disability, disuse and probably depression. In our experience, this pattern is more common in people who are afraid of pain and re-injuring tissues and for people who are 'passive copers'.
The common feature of both graphs is that the eventual activity limit is extremely low. This activity limit is low because pain has become the master.
105 ________ J~AIN ONSET
GRAPH
I: 'DESCENT INTO CHRONICITY'
>-
I-
> IU
« EVENTUAL ACTIVITY LIMIT
..
TI M E
GRAPH 2: 'BOOM-BUST'
. - FLARE-UP OCCURS
---------->-
------------------------ _____________
~PAINONSET
I-
> IU
INCAPACITATED ----.
-----------------------------------------------
---
« EVENTUAL ACTIVITY LIMIT
TIME
..
1
;.
p<.. -~
3
[,,...'
rrJ q.l r'
Elxp; ~
nn
-Il{
-,[)I)n
,UA J .1:
r.
rO:l
1e
;11
t
V
r
L..:....
!',.IuF'-
r
',7
r r l..'~H.
Recap
Modern management models incorporate the
}h
current sCientific knowledge and do not focus
ld
'r
tlT
solely on tissues.
r'
, c
t.
r .-, _TTL r
r q.{!',~ c - 11
',( T'i'
..,r I
I]]
~'l.!
'rJ.
P'
These models recognise the importance of
fl'
alarm system sensitivity, fears, attitudes and beliefs in a chronic pain state.
yo
How you understand and cope with pain l..f1 t ,(
rJ.
if 1 _ l:.1r ('-' rr
rr
affects your pain as well as your life.
r if
Many people with persistent pain relate to the
'1:,lT'
'pain as your guide' or 'boom-bust' cycles. While understandable, these cycles are not helpful and lead to drastic limitation of activity and meaning in life.
2
4
.[
w
/-': 'I
t(
(. :.1 !:., .. c
lr r
t
n
t .• r
1~
r
A
11.
r
-'-t t
b
1
Tt
t t
) (
co
r-t
0
ex)
~
~
0 H
~
~
H
rrj
;j
C)
o,..-{
0
CI.l
,..--.i
ro
o,..-{
+=l
~
Q)
CI.l CI.l
Q)
~ Q)
s
Q)
IQ.Q
ro ro~
~
u.l
+'
u.l
OJ
+' CIJ
CIJ
p.,
~
0
CIl
'd 1=1 cU
~
0 H 0
'';
'';
CIJ
0
~
.S cU p.
OJ
'd 0
JZl
d 0
1=1
0
H
cU ...., p.
S
'';
H OJ
CIJ
.!< />
1=1
1=1
_0
.....0
CIJ
~s
'';
+'
OJ
;::J cU
0 OJ
.0 1=1
'< />
H
.r<
CIl
;c1 0
;::J
1=1
H
.0 CIl '';
...., 1=1 OJ
S OJ
OJ
cU
.c:...., ...,
s
.c:...., 5
cU
1=1 cU
0
.c:....,
1il '3 g:~ .ScU
0
CIl
.g -
.S S 1il 0
.~
0
'H
.c: cU
.±::
CIJ
..... OJ +' 0 .c: 1il .~ 1=1 OJ .c:..., P. <2 OJ ...., H OJ
CIJ
cU
1=1
OJ H 0 '';
b ~
0
...., u.l OJ
...., ;::J
1=1
0
1=1
....,
CIl CIJ
s
OJ OJ
5
~
Ii
' ';
~ ~
rD '';
cU
OJ H
CIJ
~
'd
~
~
OJ
.r<
CIl
OJ
.c:~
CIJ
OJ 0
1=1
.....
~
OJ H OJ OJ
~
0 CIl
1=1 OJ
CIl
IlO
H
OJ
.--<
'd cU
'';
.--<
CIl
0
ai
cU
~ ......
CIJ
OJ
0
OJ
£cU
.s
0 H
CIJ
'M
;::::I
<2
.&
u.l
IlO
.SOJ cU
OJ H
OJ
0
P.
.--<
OJ
H OJ
'd 'rl
~
~
~ OJ H
0 iJ;,
rD OJ
s
'';
~
...., OJ H
~
·rl
0
0
u.l
OJ
0
1=1
CIJ
H +'
OJ
~
a 1il
u.l
OJ
CIJ CIJ
;::J
'';
OJ
.--<
OJ H
H OJ
.....CIl OJ H OJ
CIl
.c: ;::J
0
;::J
H
c8 0
OJ
oJ
IlO
'd OJ
~
.--<
;J Ii
.....0 ;::J
1il0
OJ
'd 'd OJ
CIJ
cU
..I? ~ ..... b
....,;::J
cU
......
~
s
OJ
S
~ cU
~
'd IlO
1=1 ''; 'd 1=1
CIl
cU ....,
OJ IlO
1=1-
.!< />
0 ~
OJ ...... ~
'd
cU
~
'd
~
;::J
'd
H OJ '';
0
'';
0
'1Qb 0 ......
~0 til 'r; -aOJ 0
cU
......
.c:...., ~
OJ
E @ ~ ...... ~ ~ tf
;::J
'§
0 ...., 0
1=1 .r< ....,
1=1
OJ ....,
1il .c:co OJ
'd OJ ......
1=1
CIJ
OJ
.0 CIl
.~
'd 1=1 ....,cU CIl
H OJ
'd
.c:....,
P. cU
.0 'd
.!< />
...;
i
~
CIJ
:;::1
OJ
'p:
'd
0
H
p.
p.
H
.!< />
OJ
§
0
'';
'd
rD
s CIJ
'';
1=1 cU
.c:0 Q)
S
.c:....,
P.
H OJ
.c:...., .~ OJ
'd
0
1=1
~
OJ OJ
1il tl 0 @ .r<
0
CIl CIJ
OJ
OJ
~
IlO
H
Q)
'd
;::J
0
.c:....,
.2....,
~
E
0
P.
H
§
'd
CIJ
·rl
p. cU
CIJ
cU
.c:
CIl
p.,
CIJ
OJ
~
CIJ
>=l cU
CIJ
OJ H
P.
0
~
'd
P.
';j
P.
.c:....,
.ScU .SOJ
OJ
~
'd
;::J
0
OJ
'd
1ilOJ
+'
cU .~ H ..., 0 OJ rD .c:...., 1il0 1ilOJ 0 S OJ 0
CIJ
;::J .~
....,
cU
.c: c-. ....,
E-I
;::J
H
JZl
;::J
p.,
cU
~
....,
z .g OJ
CIl
~ +'
.rl
.c:...,
0
'p: ..... ...., 1=1
0
·rl
cU
H
H OJ
fit
OJ
';j
'';
0
S
~
1=1
IlO
1=1
;;j
OJ ..., 0~ S -1=1
~
til ....,
'd 1=1 OJ IlO
·rl
;::J
JZl
'd
OJ
.c: 1il ~ Ii 'd P. cU 0 5;> .~ ..., ~ CIJ .c: ...., tl H 1il0 c8;::J S H ....,OJ OJ c8
.!< />
1=1
~0 c8
OJ
'd
til
1=1 ;::J
'd
CIl
~
H OJ
cU
H OJ
.c:...., IlO
.8
;::J 0
0
S
OJ
.0
.:, 0
H
.c: CIJ
fit
p.
H
0
p.
H
'';
OJ ~ 1il OJ
0
Q)
1=1 ~
+'
.....OJ .....g:
'd
OJ ...... P.
..... S ..., 1il
OJ
'd
.....0
1il
Ii
P.
H OJ
0
.c:....,
CIJ ...... 0 0 ....,
~
'';
.c:0
S ~
~
.c:
OJ
.--<
p.
H
.....0
OJ H OJ
1=1
'd 1=1
H OJ
~
0
0
CIJ
H +'
;::J
.s
~ OJ
1il
OJ
.0 'd
~
~ .....
OJ H
fib od OJ OJ tl
'd 1=1 cU
OJ H
;c1
IlO
:2'
CIJ
€ 0
·rl
OJ
til
~
OJ CIJ
0
B
~
~
g 0
'd
H 0
OJ
;::J
§
'd 1=1 cU IlO
.S 'd
.~
0 'p: <2HcU 1? cU S 1il ~
.0 CIJ
.0
'';
OJ H
1=1
0 ....,
'IlO aJ
CIJ
co~
0
.--<
CIJ
.s
OJ
'd 1=1 ;::J 'd 1=1 cU
1=1
....,
~ SOJ
CIl
OJ OJ
1=1
.c:....,
0
'd 1=1 ;::J
cU cU
~
~
H
CIJ CIJ
H
S 5;>
.c: ~ ~ ....,HOJ 0
0
0 ....,
.0
OJ ....,0 .c:
~
til
OJ H OJ
Ii
.c:....,
b....,
.0 til
p.
1=1
0
0
1=1
CIJ
'';
CIJ
OJ ....,
·rl
IlO
1=1
OJ ~
~ 1il ES ....,CIJcU .c: ....,
.c:
0
'';
H
c8 OJ ....,
'd CIJ
OJ IlO IlO CIJ
;::J
~ OJ OJ
.0
OJ
.-i
....,CIJ
'M
OJ .c: 'p: 1ilOJ
...,0 ~ 0 cU ...,H ....,:>;
P.
OJ
1=1
OJ
+'
.c:
§
OJ
CIJ
.scU ~
ai
H
'd 1=1 cU
.....
a~
0
H
1=1 cU
0
E-I
.S .c:OJ ;::J
CIJ
~
Ii
1=1
0
.0
i3 'aJ
~
0
cU ~ p., .0
~ OJ
.r<
1il ~
P.
OJ H OJ H H
0
'd 1=1 cU
'd
1=1
.8 60 ~ c8OJ .c: H
~ ;::J
cU
CIl
OJ
P.
s ~ ...,..., E 1il
0 ....,
0
CIJ
1=1
CIJ
OJ .c:...., ,§ .S CIJ
OJ
.c: ~ ~ tl OJ cb
H
CIJ
~ OJ
.c: ~ ~ tlOJ
b OJ
0
'';
CIJ
0
'd
~
CIJ
0
0 ...., OJ
~
S
~
OJ IlO
til
~
1=1 cU
cU 1=1 cU
s s ;q
~
0
H-
.--<
1il 1? .c:...., cU
OJ
s
.c:...., 'H
'H
0
1=1
OJ IlO H OJ
0
0
6
0
OJ
0
.0
·rl
0 .--< 0
.--<
p. ~ H OJ .c: ;:::1 .c: ...., ;::J 0 6ll cU E-I 0 1=1 0 0 H 0 c8 ~ ~ .c:0 .c:0 0 .c: ;c1~ p.~
~
H OJ
CIJ
~
OJ ...... IlO
~
OJ
cU
CIJ
oJ
CIJ
.S ~cU ·rl
CIJ
cU CIJ
1=1 cU CIl
s
0
'd
OJ
......
·rl
0
Q)
~
·rl
1=1
oJ ......
p.
P.
OJ
0
OJ H OJ
cU
.c: OJ
1=1
9 OJ 0 ~ Z ......
5;>
••••••••••••••••••••••••
os
Po
....R R
.'
...osPo >: Q)
pain
6 110
Tool 1: Education and understanding The primary step in management
Bythe time you reach this point in the book, and you
Let's think about the no pain, no gain road. People talk
understand what we've been saying, you will know more
about pushing through the pain barriers. We don't support
about pain than many health professionals' . Unless
this, although for some people there is no harm in vigorous
clinicians are up to date with science, some of the notions
exercise as long as they understand any pain that is
presented in this book may be unfamiliar to them.
provoked. For example, some discomfort as you rehabilitate stiff joints and tight muscles is probably necessary. But pain is a bit like love, joy or jealousy - have you ever heard of anyone pushing through the love or joy or jealousy barrier? Maybe we should say, 'know pain, or no gain' . What about the let pain be your guide road? For most people in chronic pain this is not useful. If you were to let pain be your guide you would do nothing. Sure, it may be of some use when you have acute pain, so that you don't interfere with the healing process - but even in that situation you will not usually avoid pain altogether. To let pain be your guide usually means that you are giving in to it, making it your master, encouraging yourself to be fearful
Test yourself. The rat has a choice of
of it. You have to take control.
three roads to travel on: the welltrodden roads of 'no pain, no gain',
We go for the third way: understand pain so that you don't
'let pain be your guide' and 'the road
fear it. This is the road less travelled, but ultimately the
less travelled' . Which road will he take?
road to recovery.
III
Here are a few important things we now know
One aim of understanding the physiology of pain is
about explaining pain:
to facilitate what is called 'deep learning', in which information is retained and understood and applied to problems at hand97 , Just learning about what
1. People without any training in the health
professions or biology can understand the
to do, but not learning why, can be thought of as
physiology of pain, even though some health
'superficial' or 'surface' learning, which is when
professionals think that they can't 1,
information is remembered but not understood or integrated with attitudes and beliefs 98,
2. Learning about pain physiology reduces the
threat value of pain2 , Reduced threat will reduce
So, understand as much as you can about what is
the activation of aU of our protective systems:
causing pain, not just what you should do about it,
sympathetic, endocrine
79
and motor
94
,
This in
turn helps restore normal immune function
82
3. Combining pain physiology education with
movement approaches will increase physical capacity, reduce pain and improve quality of life 16,96,
,98,
Remember - knowledge is the great liberator!
pain
6 112
Tool 2: Your hurts won't harm you Smart thin.h.ing
Test yourself... if you have understood this book then
I' ~
you will now be able to understand that 'when I am
hurting, it doesn't necessarily mean that I am damaging myself'.
You should know that because of the ways the nervous system and brain change in order to protect your tissues, we can be confident that persistent pain does not necessarily reflect the condition of your tissues. So, if your pain has persisted for longer than tissues take to
heal, then increases in pain do not necessarily mean that you are sustaining new damage.
In the same way, recurrent pains are often protective. If you have had a recurring pain for many years, each
recurrence does not mean you have re-injured that muscle, joint, ligament or nerve. It makes more sense
scientifically to conclude that recurrences occur because some cue or set of cues has been sufficient to activate the virtual representation of the old injury. A little like your brain checking up on you - making sure your body is OK, safe and sound. Perhaps the orchestra has decided to play the pain tune to make sure it doesn't forget it.
113
So, hurt does not always equal harm. Simply by
A practical exercise:
reminding yourself of this each time you are in pain can
Let's say you are just sitting around and you feel some
help reset this system; the sophisticated name for this
pain. Think about it. Think about what you know about
strategy is 'self-talking' .
pain. Think of what may have activated the alarm systems . Reflect on what cues may have ignited the pain
But wait! This certainly does not mean that you go out
nodes in your brain. Why has the orchestra started the
and learn bungee jumping, decide to walk across town
pain tune even though you haven't touched the tissues?
or go on a ballroom dancing marathon. Your body is not
Get to know your pain.
prepared for such a big step and your already senSitised nervous system will take drastic measures to stop you Q.oing that again. In fact, when the central nervous system gets really desperate to prevent you from damaging yourself, it can paralyse your muscles ( called 'spinal shock' - it does go away) or make you faint, vomit , pass-out, whatever it has to do .
When you understand that hurt does not equal harm, we hope you also understand why your nervous system will not let you do anything more than gradually increase your activity or exercise level.
pain
6 114
Tool 3: Pacing and graded exposure PaULV..L..LV'; and ~-----:..----- ~-'1~~'
M
ovement is essential for the health of all body systems
and processes. It is the principal body function which is affected, altered and sometimes controlled by pain.
The body tissues, especially the muscles, joints and nerves are designed for, and love, activity. Movement will always be of benefit for tissues. Muscles can be made stronger
The art of graded exposure and pacing. Scoring some brain triumphs.
right throughout the life span and all the tissues can be kept happily sliding via movement. Many therapists know the term 'motion is lotion'. There are many health professionals skilled in movement rehabilitation and fitness of tissues.
If you can understand your pain, and you know that it will
not damage your tissues, you can move. Here are the basic principles that you can use as a guide lD4 . There are also helpful books that talk a great deal about pacing99 103. See
But if you are in pain for a long time, you might know you
the list of our 6 most helpful books on page 129.
need to move, you really want to move, but are 'trapped' by pain. You have to be smart here - smart activities are required.
1. Decide what you want to do more of. If you feel you
would like to do more of everything, this may seem silly. However, start by picking an activity that you particularly want to do more of, for example reading, walking, ironing, working, not wearing a neck collar, playing with the children, sitting, sleeping, driving etc. You could also consider what you need to do more of.
115 2. Find your baseline. A baseline is that amount of the
activity that you can do and know that the pain won't flare-up. A flare-up is that increase in pain, often sudden, that leaves you debilitated for hours, sometimes days, and feeling really desperate. Try running conversations like this through your mind (we have supplied some typical example answers):
How long con I walk before I ~are-up? I can walk for 30 minutes but I pay for it the next day. Can I walk for 20 minutes without ~aring up? No. I will still pay for it. Can I walk for 10 minutes WIthout ~anng up? Probably not - definitely not up hills. 5 minutes on a ~at surface? Probably. 3 minutes on a ~at surface? Definitely. So, for walking, your baseline would be 3 minutes on a flat surface. You can go through this process for every activity, or combination of activities. Remember, going out to a party or function is an activity also. 3. Plan your progression. Because you know that 'let
pain be your guide' and 'no pain, no gain' are not the ideal paths to choose, you need to plan your baseline increases in advance. Be gentle on yourself. Taking the example above, you could plan to walk slightly further each day for the next week - 3 1/2 minutes, 4, 4 1/2, 6, 6 1/2 etc. Often, time is a good measure. An alarm clock is invaluable: setting an alarm for your pre-planned
period will allow you to benefit from distraction (e.g. read a good book) without exceeding the limit and flaring up. When you have planned ahead, you will often complete the set amount of activity and be feeling really good - do not be tempted to break the plan and push on. This will lead you right into the boom-bust trap. One step at a time - be patient. 4. Don't flare up, but don't freak out if you dol
Because the alarm system is so sensitive, it is very difficult to completely avoid flare-ups. If you do flare up - do not give yourself a hard time and stress out! Remember what a flare-up is - your nervous system trying to protect you. When you flare up, it can be tempting to give up, forget what you know about pain, and seek some radical but inappropriate quick-fix treatment. Don't give up - be persistent. 5. It's a lifestyle thing. In the short term you will have to plan your life a little more. You will benefit
from seeking out 'happy activities', because they have known physiological effects on your alarm system and pain ignition nodes. Choose fun activities if you can, or do them with fun people, or to your favourite music. Challenge some feared activities when you become more confident. We know that this sounds simple. However, if you have had pain for a long time you will know how difficult it really is. This process is doing some pretty complex things to your brain. However, we know that if you stick with these principles you will gradually return to normal life and overcome your pain 16.92.96.
pain
6
116
Tool 3: Pacing and graded exposure :continued) StLJ
L' ....
t .....,ut
T hese mountain figures are a useful way of understanding
NTT (new) The new tissue tolerance line
the relationship between your pain, the nervous system
Look at the mountain on the top right. If you have had
changes that occur with persistent pain, and the brain
pain for some time, the line shifts. Your tissues are not like
retraining activities of graded exposure and pacinglO3.
they were - especially if they have sustained an injury.
Let's walk through the left side of the top figure.
Although the tissues might have healed, they may not perform quite the same way. More importantly, you have
TT (initial) The old tissue tolerance line
not used the tissues as much or in the same way since your
Before your pain started, your tissues were fit and healthy.
pain started. They are unfit, weaker, more easily fatigued.
There was a certain amount of activity that you could do
This is one reason you shouldn't just push through pain,
before your tissues would fail in some way. Most tissues are
dose up on analgesics or climb a steep mountain for example.
damaged by reaching the tissue tolerance line too quickly (e.g. falling, lifting a heavy weight, a car accident).
NPBP (new) New protect by pain line
Sometimes, this line is reached slowly while you are
Your alarm system and pain ignition nodes are sensitised.
distracted (e.g. working or training).
You have pain at very low levels of activity - perhaps all the time. Your brain is really looking out for you. Take notice of
PBP (initial) Protect by pain line
the size of the protective buffer between the onset of pain
Danger sensors are activated before damage occurs and
and the new tissue tolerance line. If you progress slowly, it
your brain is alerted. Usually, the pain ignition nodes are
will be impossible to re-injure the tissues because it will
activated, the neurotag for pain is produced and it hurts.
hurt too much to even get close to this line.
Pain motivates you to stop or change the activity to get your tissues out of danger. A great system. You could go
FUL The flare-up line
further or climb higher, but it gets dangerous.
BL The baseline from which to begin activity
117 KEY TT
(initial) old tissue
Superhuman effort (dangerous)
tolerance line PBP
(initial) protect by pain line
TT PBP
NTT
NPBP new protect by pain line NTT
FUL BL
new tissue
NPBP
tolerance line FUL
flare-up line
BL
baseline
AFTER INJURY
BEFORE INJURY
And now plan your 'training'. Let's walk through the first of the small mountains in the figure below. A. Starting below the
flare-up line, gradually
B. The flare-up line will
slowly lift along with your
C. The protect by pain line will slowly lift - the
D. The tissue tolerance line will also lift - this is one
increase your activity,
training level (this is
sensitivity of the system
of the beautiful
planning steps in
because you are training
reduces.
properties of highly
advance: 'always do more
your brain, reducing the
adaptable beings - the
than you did yesterday,
perceived threat, accessing
tissues get stronger,
but not much more' .
the virtual body in a
fitter, better controlled.
non-threatening way).
N TT FUL BL N PBP
PACING & GRADED EXPOSURE
pain
6 118
Tool 4: Accessing the virtual body G...,u'',&. ...... J t..,l, .LV~},.j
T he virtual body in the brain can be exercised just like the
Of course, while you are experimenting with movements
actual body. The techniques of pacing discussed in the last
there could be some pains evoked. This is OK - remember,
few pages can be used for actual and/or virtual body
if you understand your pain and know that it won't harm
exercises. The good thing about virtual body activities is
you, then there will be minimal stress responses.
that you can do them anywhere, you can integrate them into daily life and you don't even have to get a sweat up.
For the purpose of this exercise, we have selected the
No gym fees either.
frequently painful activities of bending forwards and turning your head. Let's see if we can work out together
Virtual body exercises are like retraining the orchestra to make it play more harmonious notes, to exercise the trumpets without the strings interfering, to revive old tunes not played for years and to compose some music for the future. The movements aim to activate brain areas that are usually activated in a pain experience, but without igniting pain (Le. the pain neurotag)B6.104. In section one we discussed how powerful context is in the pain experience. Context changes can also be used in therapy. For example, you could perform a movement in a different to usual position or environment, or you could look or not look at the moving part. Once you get the idea, you will be able to invent endless virtual body exercises that particularly suit your needs.
what can be altered.
119 BENDING FORWARDS
2. Alter gravitational influences
We are aiming here to re-learn the movement of bending
Sitting on the floor with your legs straight out in front of
forwards without the orchestra snapping into the pain tune.
you is the same body formation as lying on the floor, face up, with your legs in the air, or standing bent over at the
1. Imagined movements - activate the brain
waist, leaning on a table - it's the gravitational force that's
neurotags but don't move the actual body
different in each case. Changing gravitational influences
Imagined movements activate many of the same brain
allows you to run brain representations of the movement
areas as actual movements. If you think about the
in similar but slightly different and novel ways.
movement you know to be painful, or watch someone else perform that movement, movement neurotags in the
If you lie on your back and pull your knees to your chest
brain will be activated but the pain neurotag probably
(one knee, if it's too sensitive to do both) - the back has
won't. Sometimes, if your pain is very chronic and severe,
been bent in the real and virtual body. You could try it
eg106
even imagined movements can be painful
,
in which
lying on different surfaces too (e .g. cold floor, warm rug),
case you could initially imagine performing part of the
just for some different inputs into the brain. Brains love
movement. What you are doing here is helping the
variety. If this is painful, perhaps just lying flat on your
orchestra to playa gentle movement melody without
back on the floor and flattening your back with your
playing its accompanying pain tune.
knees bent is your appropriate level of activity. You can
....... ..... ~..... .. .........' ... ... ... . ...... - - ....... '
_
flex forward while sitting on a chair. Performing movements in water is another way to alter gravitational influences. Altering gravity also alters levels of movement security. There is greater security leaning on a wall and bending than bending without support.
pain
6 120
Accessing the virtual body ( continued)
3. Add varying balance challenges
5. Alter the environment of activities
The forward bending movements could be
You could perform forward bending movements in
performed sitting on a fitness ball and bending
the comfort and security of your home, or be
forwards, rolling the ball under you as you bend.
adventurous and do them in the park like the Tai
A further progression would be to bend forwards
Chi groups, or even at work or where the injury
with your arms up to the ceiling or pointing down
happened. Performing movements in water allows
to the ground and moving your legs to one side
environmental inputs from variations in balance,
and then the other. These inputs will also provide
temperature, smells, other people around and
some virtual body changes via distraction.
wearing different clothing. You can stand in a pool up to your chin in water, lift one knee up
4. Vary visual inputs
and pull the knee towards your chest. This will
Performing a movement with your eyes closed
bend your back a little, but the virtual back
usually means a greater challenge for the virtual
bending in your brain will be very different to the
body. If you can perform a movement, say bending
one you ignite when you bend your back in the
forwards from the waist on a chair without
therapist or doctor's office.
igniting a pain neurotag, try to look at your body while you are doing it, so perhaps do it in front of or side-on to a mirror. The visual input to the brain reinforces the message that a movement, which the brain 'knows' to be painful, doesn't have to be.
121 6. Do the movement in different emotional states
conducive to getting moving and changing rhythm
We tend to put exercise and activity off when we are
would be useful. Doing artwork which allows you to go
feeling a bit down, but if you were to perform activities
into aspects of the pain experience but without igniting
such as those listed above in various emotional states, it
the pain experience would be therapeutic in itself.
would give the virtual body a richer context of
Distraction is not a simple pain reliever - combine it
representations in which to run. You are now teaching
with some creative activities for added power.
the orchestra to play some pretty sublime and new -age tunes. The better the orchestra becomes, the more
6. Plan functional activities which involve bending
harmoniously it will play together and the more it will
the back
be able to remember new tunes. Also the less it will tend
When a part of your body hurts, your brain will accept
to snap into that old familiar pain tune.
movements that it knows are familiar and necessary to your comfort and survival - meaningful movements.
7. Add distractions
While some meaningful movements can hurt if they
Distraction is a powerful way to disable the pain neurotag.
bring back memories of pain, many are gratefully
Distraction removes one of the key ignition nodes (see
accepted by the brain. We flex our backs when we lie on
page 39), the node which is activated when you
our sides to go to sleep (on either Side). We bend our
concentrate or focus on something (such as pain). You
backs to put on shoes, to pick something up off the floor
could use mUSiC, mediation, visualisation or you could
and to speak to children.
even alter the environment of exercise. Music which is
[VJ ~
pain
6
122
Accessing the virtual body (continued)
9. Break down functional movements that involve
10. 'Sliders'
the back
'Sliders' are techniques that encourage total body
People who have persistent pain lose their quality of
movement SB • An example of a slider is when you lie on your
movement - they perform activities such as rising from a
back with your knees bent and feet on the floor, and flatten
chair or picking up an object from the floor in very
your back (thus flexing it up a little) and at the same time
regimented ways. See if you can perform the activity in
tilting your chin upwards. This allows distraction plus
different ways. For example, when you rise from a chair,
movements which are unlikely to aggravate sensitive neural
try it with one foot forward then the other, lead with the
tissue in your low back. Another slider is to sit upright in a
head, with eyes open or closed and try performing the
chair and sag your back, hold under your thigh and extend
routines at different speeds. Feed some quality varietal
your knee while tipping your head back. Think about
movement to the brain.
kicking your head off! 11. Perform movements with neighbouring tissues in a 'friendly' state Sitting in a chair, if you bend forwards and have your chin
~
tilted forwards it will slacken some of your nerves in the back. Bending forwards when sitting means that some of
,
SLIDERS
the tension is taken away from the tissues in your hips and legs. You may need to look at page 114 to incorporate these movements into a pacing process that will work for you without making your pain flare up.
123 12. Playing with your 'glitches'
Here are a few specific head turning examples:
Glitches are the ways we have all learned to wriggle and
• If you sit on a swivel chair, look at a fixed object and
adjust when we perform a movement. They are often
rotate your body while looking at the fixed object, you
caused by memories of painful movement. For example,
are performing a neck rotation but in a different
you may know that the best way to bend forwards is to hold your back in a certain position, lean on your knee etc - methods that you use as a helper to make the movement easier for you. These glitches may be little memory boosters to the pain neurotag. See if you can work out ways of performing a movement without the
context. • If you fold your arms and shrug your shoulders a little you are slackening nerves which may enable a better head rotation. • Stand close to a wall and write your name or play an
glitch. Sometimes sliders (moving another part of the
imaginary game of noughts and crosses on the wall
body when the glitch occurs) can remove them. Maybe
with your nose. Try it standing on one leg, or with
you can take a thoughtful approach to it and ask
your eyes closed.
yourself - 'do I really need to have that glitch' and try and move without it.
• You could rotate your head with your tongue, jaw and mouth in different positions. • It is usually much easier to turn your head when you
13. Let your mind go
You could bend on the pew or on a bar stool, bend when there are different smells or playing the fool, bend with the arms up or by your side, bend when it's noisy or holding your breath, or do it in the nude or in your SundfliY best. TURNING YOUR HEAD
are lying down. • You could turn your eyes to a point on a wall and then follow them with your head. • Make noises while you perform movements . • Learning to juggle may help your neck as well. Can you see why?
If you use the categories above, you should be able to construct virtual exercises for any part of the body. Simply - work out ways to move and use the painful part of your body without activating the pain neurotag. Turning your head often hurts if you have a painful neck.
Make the neurotag curious, make it wonder 'what's next'. You be the master.
1
3
Rer 3p
• All pa.ln experiences 'l.l'e a norllal response
what your bra!' thirJ:.s is a The a:nount of ner:.'l?sa.·~ly
pc'~n
'elatE: tl' W:.E:
Ti..lsue damage
,Q
~hreat
you exper _~:-~ 'E:. does aIr Iu.~t
of tlSE
at
in li.1rr~l'a'iOl-. which
rF.l1tcls
r..any SEc 'lory
,>11
I'hu.J'to.T lLnb
pa,-~ ,.:~ v~r
v~.tt.al ~b
1
uhe bra.
a
•
ne1..:o:' 'S
E.olp.ly
0:'1
T'>el'e
IILO( < ')
IT 11'9
sfnslt'vEI E2r I',
uP'. m
p~ 0:
r.
)1nS
l Il.
rpnITC E ~
0
•
oJ.
',. r 9.ndE
t:.L.... iU(~i
enj'i
depend';
o~
11
the blc (ld supply
the ti SllUe n: 'T(..
'If
ld
I.e
t 'ill
t.II over ';he borJy
• When thp excit.ement level witrl. n ' neurone reaehes the critical level, a n,jES8.gP IS SEnt towardE the (PIC1al cord • When a. danger 'l'('s(£..ge reaches the 'lpinal cord it ca;,'les 'Elleasp G' (1{C tatory ChE miC'll>; Into the syna.pse • Sensors.n ';he dangE.r
e'1ngllu.'
rp.cep~L'I'l.
')'8,(,)
(2.n bl;iJTh 'tte
N m'l'Ll y, pab). .ui',kttld b.v
';'E l' m('~,la~'_'S 'rOI'. ~h€' I.E rvEi;; f ,~
n: '!,G
[fer neW'onll 'lre
rctlV'l.tnd by tholln excitatory ch8mlcals tV'c' when the
r;xl)i~e~rer.t :'~vP:
of the
dsn'Se~
m6<.::enger nf'Urone reaches t-le c'-'.tlCal Ev('. ~.
•
danger message IS sent ';0 the brE'in
Tl- p message
II?
processed thrC':..ghout tl'.., bra n
end i' the br!J.jn cvnclude'l yot. are in danger 'k'.d
1JThen ,.'( in becom6~
PFJrs~
'lts 'hFJ dJ.Lger 'll'l.l'T ,;y&';em
'Op'
wi~h fl8.1n
Ur
~, }~pf'
,
lh
g'l • ~'
r 'bnl
'f 1
bUE';' C y' .s
,iE:1'.,u,lr.dabI8, t'.eef' eye
c.1r
C
l;!ld~,)
circE.t1c
rnt.
E: C.1C,
L4m1~d.tio:
l
f'
Recap
• Education and understanding are critical for you to overcome pain and return to life.
mo:. E' 'en, itive
• Th8 dang'.!' mE;t:.Jenler r.F,ll.l'One become:, more
• A key is to understand why your hurts won't
excite.ble tnd 'ILan' Ifwctt...' E2 [10: €' Ltcln ,on fo;:
harm you and that your nervous system now
eXc.ltatory chemic. '
uses pain to protect at all costs, not to inform
T1:.P. br'l!n stau tIJ ac.tlvatlLg IlE .I·OllF' th<1t
t.-,,, .jor'lal
horn of the r,PUla. cor'1.. • Rellp'1nse bYEt',n::S bFJI)ome more lILV Jlved and st,art contributing Lo
~hE1
prc,':l.errl
con~rihu.t·n€
to thFJ problem
the neurotae. for pc... n (,h8 'patn tune
to t,he danger message aPl'iving at
activities and involvement in life.
~he
danger-reducing chemicals. • You can quickly learn to exercise the virtual
• • T'J.e brain n.dE'pts tD become bett.::;:· tt _,rOL ueing
::l8~
• By being patient and persistent, you can use
• Purposefully seek out activities that produce
rh.oughts and bel1eft become more invc.lved and start
you about damage.
smart activities to gradually increase your
body as well as the actual body. • By mastering your situation and then planning
• Dangel' &enBOrS in the tlSE-ueS contribute less and together' to get you out of d<1nger
Wh:le
[§]
vou need to tElte t.ctio:-J, It will produce patn • The brain activates Jeveral Lysteml:i that work
i c.!.!'
vlTf111 a· your IS.'
1.,
activity 1.ndT.eani:rt!1 •.'1 Ii e
F,ec:.'
release FJxcitatory ch 1'I icals at meIlSp.~
ndt'rst~.'1
yc .r pain
M U'y p,'0p18 w.tr. pE;r, iEten, P;1L Ire tt;) to t. ,p.
4 'lca~tered
How you
'pal' dE v
1' It';
fo.lcwr a pn.rtieli. 'l.r Pt·,tt,3r;1.
Dar..f,Er lE1n5U'S are
r port'1I1ce Jf
du.!'<,c dc
Recap
I
,,:t'vit.'l, foar' attLt ,'c. and
bF' ' lfl in a r:h', - ir: Pill llt'1',f
affe>~'1
he'U
rec( bIl1l:'E ';hE,
I 'lL
Tl.€I r,8riph€'r1:L ne>IV,'3 kl'lm ;~fV8' 'l.rlri t. J
dt p?,E l'
2
uI'FlueFl.
al,' r 'lY-,t£'
T!~~uE' h~allng
cr
r:UE>o,
Mod81'-. mtna6J: ner:ot l1HJdol, inco!';Jorate U.e C'..ll'rent (.(-Lfntl'lc k lrl'Nledgll lnd do net foC',,!
realing.
• The c()nstructio:. 0; t1-J.e pam €'xperience of th€'
uhe
C2·UE 88
R.ec,a.p
directly f.etiYltes dr;mger sensor'l and rr'l.k'lR
Ir:ofl( r rnu.tro' in thq
~E
d lmag€'.
bri!.::
5
Recap
bratT'
your return to normal life, you will be able to do so. The research shows that it can work.
125
References 1.
Moseley, G.L., Unravelling the barriers to reconceptualisation of the problem in chronic pain: the actual and perceived ability of patients and
13. www.Ba.yer.com. On-line Harmony No. 40. 14.
Moseley, G.L., P.W. Hodges, and M.K Nicholas,
reorganisation after amputation. Brain, 1998. 121:717-724.
preparation. J Clin Pharmacol, 1982. 2:245-248.
neurophysiology. J Pain, 2003. 4:184-189. 15.
Wall, P.D., Pain, the Science of Suffering. 1999,
26.
neurophysiology education in chronic low back
16.
the phantom limb. Neurosci Letters, 1995.
3.
Blyth, FM. and et al., Chronic pain in Australia: a
4.
Bhattacharjee, N. et al, A wooden foreign body in
individual pain physiology education:
The Times, 17 Feb 2003, p. 5, London.
6.
Beecher, H., Relationship of the significance of the
17.
7.
8.
Carlen, P.L., et al., Phantom limbs and related phenomena in recent traumatic amputations. Neurology, 1978. 28:211-217.
18.
9.
www.sharkattacks.comJnewsl.htm. 2003.
10.
Bainbridge, D., Making babies: the science of
11.
Levine, FM. and L.L. De Simone, The effects of
28.
a regional pain centre. Pain Clinic, 1995. 8:323-332 . 29.
Flor, H. The image of pain. in Proc Pain Soc (Britain). 2003. Glasgow, Scotland.
21.
30.
74:79-91. 22.
geographically defined general population: Studies localization. Cl1n J Pain, 1993.9:174-182. 31.
characteristics and relationship to pre-amputation
Soc Sci Med, 1984. 19:1331-1337. 32.
23.
Melzack, R., et al., Phantom limbs in people with congenital limb deficiency or amputation in early
Editors. 1994, Churchill Livingstone: Edinburgh.
circumcision on pain response during subsequent
33.
24 .
Flor, H ., et al., Phantom limb pain as a perceptual
R. Melzack, Editors. 1994, Churchill Livingstone:
correlate of cortical reorganisation following arm
Edinburgh.
amputation. Nature, 1995. 375:482-484.
Unruh, A.M., Pain across the lifespan, in Pain. A Textbook for Therapists, J. Strong et.al., Editors. 2002, Churchill Livingstone: Edinburgh.
34.
Zborowskl, M., Cultural components in responses to pain. J Soc Iss, 1952.8:16-30.
childhood. Brain, 1997. 120:1603-20.
Spanos , N., S. Carmanico, and J. Ellis, HypnotiC
Taddio, A., J. Katz, and et al, Effects of neonatal routine vaccination. Lancet, 1997. 349:599-603.
pain. Pain, 1985.21:267-268.
Merskey, H., Pain and Psychological Medicine, in
Craig, KD., et al., Developmental changes in infant pain expression during immunisation injections .
Jensen, T.S., et al., Immediate and long term phantom limb pain in amputees: incidence, clinical
Andersson, H.I., et al., Chronic pain in a of differences in gender, social class, and pain
DaviS, R.w., Phantom sensation, phantom pain and stump pain. Arch Phys Med and Rehabil, 1993.
Schumacher, G., et aI., Uniformity of the pain threshold in man. SCience, 1940.92:110-112.
experimenter gender on pain report in male and
20.
Benbow, S., L. Cossins, and D. Bowsher, A comparison of young and elderly patients attending
female subjects. Pain, 1991. 44:69-72.
pregnancy. 2000, Cambridge, Mass.: Harvard
analgesia, in The Textbook of Pain, P.D. Wall and
129, J. Sandkillller, B. Bromm, and G.F Gebhart, Editors. 2000, ElSevier: Amsterdam.
induced pain. Pain, 1991. 44: 45-50. 19.
University Press.
The Textbook of Pain, P.D. Wall and R. Melzack,
12.
Bayer, T.L., P.E. Baer, and C. Early, Situational and psychophysiological factors in psychologically
Jensen, M., Magnetic resonance imaging of the lumbar spine in people without low back pain. New Eng J Med, 1994. 331:69-73.
Smith, W.B., R.H . Gracely, and M.A. Safer, The meaning of pain: cancer patients' rating and recall
Flor, H., The functional organization of the brain in chronic pain, in Progress in Brain Research, Vol
of pain intenSity and affect. Pain, 1998. 78:123-9.
wound to the pain experience . JAMA, 1956. 161:1604-1613.
27.
J Man Manip Therap 2003. 11:88-94.
Bulletin, 1997.23:63-65 5.
201: 262-264.
a successful treatment for chronic low back pain.
prevalence study. Pain, 2001. 89:127-134.
the neck. Bangladesh Medical Research Council
Moseley, G.L., Joining forces - combining cognitiontargeted motor control training with group or
Knecht, S., et al., Cortical reorganisation in human amputees and mislocal1sation of painful stimuli to
London: Weidenfield & Nicholson.
A randomized controlled trial of intensive pain. Cl1n J Pain (In Press), 2003.
Knecht, S., et al., Plasticity of plastiCity? Changes in the pattern of perceptual correlates of
Buckalew, L.W. and KE. COffield, An investigation of drug expectancy as a function of colour, size and
health professionals to understand the
2.
25.
35.
Bates, M.S., T.W. Edwards, and KO. Anderson, Ethnocultural influences on variation in chronic pain perception. Pain, 1993. 52:101-112.
pain
126 36.
48.
van Tulder, M. et al, Spinal radiographic findings and non-specific low back pain. Spine, 1997. 22:427-434.
61.
Craig, AD., Functional anatomy of supraspinal pain processing with reference to the central pain syndrome, in Pain 1999 - An Updated
49.
Hitselberger, W.E. and R.M. Witten, Abnormal myelograms in asymptomatic patients. J Neurosurg, 1968. 28:204-206.
62.
Review, M. Max, Editor. lASP Press: Seattle.
50.
Hardy, J.D., H.G. Wolff, and H. Goodell, Pain Sensations and Reactions. 1952, New York: Haffner Publishmg.
37.
38.
Melzack, R. and PD. Wall, The Challenge of Pain. 2nd ed. 1996, London: Penguin.
39.
Peyron, R, B. Laurent, and L. Garcia-Larrea, Functional imaging of brain responses to pain.
51.
Taylor, J.R and B.A Kakulas, Neck Injuries. Lancet, 1991. 338:1343-1346.
A review and meta-analysis. Neurophysiol Clln,
52.
Sunderland, S., Nerves and Nerve Injuries. 2nd ed. 1978, Melbourne: Church1ll livingstone.
53.
Devor, M. and Z. Seltzer, PathophySiology of damaged nerves in relation to chronic pain, in The Textbook of Pain, PD. Wall and R Melzack, Editors. 1999, Church1ll livingstone: Edinburgh.
2000. 30:263-88. 40.
Ingvar, M., Pain and functional1maging. Philosophical Transactions of the Royal Society of London. B, 1999. 354: 1347-1358.
41.
42.
Edwards, F.A, Dancing dendrites. Nature, 1998. 394:129-130.
54.
Loeser, J.D., Pain due to nerve injury. Spine, 1985. 10:232-235.
55.
Butler, D.S., The Sensitive Nervous System. 2000, Adelaide: Noigroup.
plasticity 1h developing human cerebral cortex. Americ J of Mental Defic, 1984. 88:488-496.
56.
Butler, D.S., Moblllsation of the Nervous System. 1991, Melbourne: Church1ll Livingstone.
Coggeshall, RE. and S.M. Carlton, Evidence for
57.
Fukuoka, T., et al., Change in mRNAs for neuropeptides and the GABA(A) receptor in dorsal root ganglion neurons in a rat experimental neuropathiC pain mode!. Pain, 1998. 78:13-26.
Kotulak, R., Inside the Brain. 1996, Kansas City· Andrews McMee!.
43.
44.
Huttenlocher, PR., Synapse el1m1nation and
an inflammation-induced change in the local glutamatergic regulation of postganglionic sympathetic efferents. Pain, 1999.83:163-8. 45.
Lund, J.P, et al., The pain-adaptation model: A discussion of the relationship between chronic musculoskeletal pain and motor activity. Can J Physiol Pharmacol, 1991. 69:683-694.
46.
58.
Jones, M.G., J.B . Munson, and S.w. Thompson, A role for nerve growth factor in sympathetic sprouting in rat dorsal root ganglia. Pain, 1999. 79:21-9.
herniation. Spine, 1990. 16:674-678.
59.
211:210-216. Bogduk, N., The innervation of the intervertebral discs, in Grieve's Modern Manual Therapy, J.D . Boyllng and N. Palastanga, Editors. 1994, Church1ll livingstone: Edinburgh.
60.
Howe, J.E, J.D. Loeser, and W.H . Calvin, Mechanosensitivity of dorsal root ganglia and chronically injured axons: a physiological basis for radicular pain of nerve root compression. Pain, 1977. 3:25-41. Hu, S.J. and J.L. Xing, An experimental model for chronic compression of dorsal root ganglion produced by intervertebral foramen stenOSiS in the rat. Pain, 1998.77:16-23.
Michaelis, M., M. Devor, and W. Janlg, Sympathetic modulation of activity in rat dorsal root ganglion neW'OIlS changes over time following peripheral nerve injury. J Neurophysiol, 1996. 76:753-63.
63.
Neary, D. and RW. Ochoa, SUb-clinical entrapment neuropathy in man. J Neurolog Sci, 1975. 24:283-298.
64.
Bear, M .E, B.W. Connors, and M .A Paradiso, Editors. Neuroscience: Exploring the Brain. 2nd ed. 2001, Lippincott, Williams and W1lk1ns: Baltimore.
65 .
Kandel, E., Nerve cells and behavior, in Principles of Neural SCience, E. Kandel, J. Schwarz, and T. Jessel, Editors. 2000, McGrawHill: New York.
66.
Abbott, B., L. Schoen, and P Badia, Predictable and unpredictable shock: behavioural measures of aversion and physiological measures of stress. Psychol Bull, 1984. 96:45-71.
67.
Torebjork, H. and J. Ochoa, Pain and itch from C-fibre stimulation. Soc Neurosc Abstr, 1980.
68.
Wall, PD. and R. Melzack, eds. Textbook of Pain. 4th ed. 1999, Church1ll Livingstone: Edinburgh.
7:228.
69.
Doubell, T.P, R.J. Mannion, and C.J. Woolf, The dorsal horn: state dependent sensory processing, plasticity and the generation of pain, in Textbook of Pain, PD. Wall and R Melzack, Editors. 1999, Churchill Livingstone: Edinburgh.
Mixter, W.J. and J.S. Barr, Rupture of the intervertebral disc with involvement of the spinal canal. New Eng J Med, 1934.
47.
Elbert, T.C., et al., Increased cortical representation of the fingers of the left hand in string players. SCience, 1995.270:305-307.
Saal, J.S., et al., High levels of inflammatory phospholipase A2 activity in lumbar disc
70.
Flor, H., et al., Extensive reorganlsation of primary somatosensory cortex in chronic back pain patients. Neurosci Letters, 1997. 244:5-8.
71.
Pascual-Leone, A and E Torres, Plasticity of the sensorimotor cortex representation of the reading finger of braille readers. Brain, 1993. 116:39-52.
127 72.
Byl, N.N. and M. Melnick, The neural consequences of repetition: clinical lmplications of a learning hypothesis.
83.
J Hand Therap, 1997. 10: 160-174. 73.
74.
Price, D.D., Psychological Mechanisms of pain and analgesia. Vol. 15. 2000, Seattle: IASP
84.
76.
86.
Nachemson, A.L., Newest knowledge of low back paln. A critical look. Clin Orthop, 1992.
Thousand Oaks: Sage Publications.
279:8-20.
diseases, and coping. 1998, New York:
87.
Waddell, G., The Back Paln Revolution. 1998, Edinburgh: Churchill Livingstone.
88.
Wallis, B.J., et al., The psychological profiles of patients With whiplash-associated headache. Cephalalgia, 1998.
Martin, P., The Sickening Mind. 1997, London: Harper-Coll1ns. Ader, R. and N. Cohen, Psychoneurolmmunology: conditioning and
18: discussion 72-3. 89.
Melzack, R., Paln and stress: a new perspective, in Psychosocial factors in paln,
Vlaeyen, J.WS. and G. Crombez, Fear of movement/(re)1njury, avoidance and paln disability in chronic low back paln patients.
stress. Ann Rev Psychol, 1993. 44:53-85. 79.
Moseley G.L., M.K. Nicholas and P.W. Hodges, Does anticipation of back paln predispose to
Lovallo, W.R., Stress and Health. 1997,
Sapolsky, R.M., Why zebras don't get ulcers:
95.
Watkins, A., Mind-body Medicine. 1997, New York: Churchill Livingstone.
96.
Moseley, G.L., Physiotherapy 1s effective for chronic low back paln. A randomised controlled trial. Aus J Physioth, 2002. 48:297-302
97.
Sandberg, J. and Y Barnard, Deep learning is difftcult. Instruc Sci, 1997. 25:15-36.
98.
Evans, B. and L. Honour, Getting inside
back trouble? Braln, 2004 (In press).
WH. Freeman and Co.
78.
Moseley, G.L. and P.W Hodges, Loss of normal
Clin J Pain, 2004 (In press).
an updated guide to stress, stress-related
77.
Euro J Pain, 2004. 8:39-45.
Kendall, N.A.S., S.J. Linton, and C.J. Maln,
Compensation Insurance Corporation of New Zealand and the National Health Committee.
change during an education intervention in
151:262-271.
associated With non-resolution of postural control after experlmental back paln.
85.
Moseley, G.L., Evidence for a direct relationship between cognitive and physical people With chronic low back paln.
variability in postural adjustments is
term disability and work loss. 1997, Well1ngton: Accident Rehabilitation &
94.
the trunk muscles. Exp Braln Res 2003.
Press. 223.
Guide to assessing psychosocial yellow flags in acute low back paln: risk factors for long
75.
Hodges, P.W, G.L. Moseley, A. Gabrielsson, and S.C. Gandevia, Experlmental muscle paln changes feed forward postural responses of
knowledge: The application of EntWistle's model of surface/deep processing producing open learning materials. Educ Psychol, 1997. 17:127-139. 99.
Nicholas, M., et al., Manage your Paln. 2000, Sydney: ABC Books.
100. Gifford, L.S., ed. Topical Issues in Paln. 1998, Nor Press: Falmouth. 101. Strong, J., Chronic paln: the Occupational Therapist's perspective. 1996, New York: Churchill Livingstone.
Man Ther, 1999. 4:187-195. 90.
R.J. Gatchel and D.C. Turk, Editors. 1999, Guildford Press: New York.
Higgs, J. and M. Jones, Clinical Reasoning in the Health Professions. 2nd ed. 2000, Oxford:
102. Wittlnk, H. and T.R. Michel, ChrOnic Paln Management for Physical Therapists. 1997, Boston: Butterworth-Heinemann.
Butterworth-Heinemann. 103. Gifford, L.S., ed. Topical Issues in Paln 3.
80.
Watkins, L.R. and S.F. Maier, The paln of
91.
being sick: lmplications of lmmune-to-braln communication for understanding paln. Ann Rev Psychol, 2000. 51:29-57.
81.
92.
Watkins, L.R., S.F. Maier, and L.E. Goehler,
Morley, S., C. Eccleston, and A. Williams, Systematic review and meta-analysis of
Immune activation: the role of pro-inflammatory cytokines in inflammation,
randomiZed controlled trials of cognitive behaviour therapy and behaviour therapy for
illness responses and pathological paln states.
chronic paln in adults, excluding headache. Paln, 1999.80:1-13.
Paln, 1995. 63:289-302. 82.
Lazarus, R.S. and S. Folkman, Stress, Appralsal and Coping. 1984, New York: Springer.
Rabin, B.S., Stress, Immune Function and Health. 1999, New York: Wiley-Liss.
93.
Snow-Turek, A., M. Norris, and G. Tan, Active and passive coping strategies in chronic paln patients. Paln, 1996. 64:455-462.
2002, CNS Press: Falmouth. 104. Moseley, G.L., A paln neuromatrlx approach to patients With chronic paln. Man Ther, 2003. 8:130-140. 105. Moseley, G.L., Imagined movements cause paln and swell1ng in a patient With complex regional pain syndrome. Neurology, 2004. 16:44. 106. Loeser, J.D., Paln and suffering. Clin J Paln, 2000. 16:S2-S6
pain
128
Index acid. . . .... . ...... 30, 48, 72, 90 lactic acid ... . .... . . . . . . . . . . . 30 ACTH. . ..... . .... ........ 86,88 action potential . . ... .. . . .... . .. . 34, 35, 37 acupuncture . . . . . . . . . . . . ........ 16 adrenaline ... . . . . . . .. . 31, 63, 84, .........
. . . . . . . . . . . . . . . . . M,M,M
age. . ....... . .. . ...... 24 bones, joints, LAFTs . . . . . . . . . . . . . . . 55, 59 nerves. . . . . . . . . . . . . . . . . . . . . . 61 alarm, alarm system .. . .... . ... 9, 12,17, 28, .. . . 29,30,32,56,63,70,72,82
all or none law . . . . . . . . . . . . . . . . . . . . 34, allodynia . . . . . . . . . . . . . . . . . . . . . . ... amputation . . . . . . .. ...... ... 13, anaesthesia .. .. . . . . . . . . . . . . . . anti-inflammatories. . ..... . . . . . . . . . . anxiety. . . . . . . . . . . ....... 67, aspirin. . . . . . . . . . . . . . . . . . . . . .. 17,
35 72 22 17 49 85 49
beliefs.
. ... . . 11, 78, 80, 84, 89, 92, 97, ........ 1 02, 106, 111 bone . . . 29, 31, 46, 54, 55, 88, 59, 62 boom-bust . . . . . . . . . . . . . . . . . . 104, 105, 115 brain imaging. . . . . . . . . . . .. . . . 23, 39, 96 burns . . . . . . . . . . . . . . . . . . . 13, 28, 56 burning pain . . . . . ..... . .. . . 66 central nervous system (see nervous system) central sensitisation . . . . . . . . . . . . . 82 chronic fatigue syndrome ..... 82, 83 chronic pain. . 15, 23, 38, 56, 76, 80 . . . . . . . . . . . . . . . . . . . . . . . . 84, 98, 102, 110 clinical decision making ... . 98, 99 compensation. . . . . . . . . . . . 50, 97 consciousness .. 28 context of pain. . . 18 , 20 , 100, 118, .. . 121, 123 cortex, motor .... 39 cortex, sensory ...... 39, 56 cortisol. . .. .. . . . . . . . 84, 86 , 8 7, 8 8 Couvade syndrome . . ... ... .. . 16 cues ...... 17-20,38,50,51,84,96,112,1 13 culture . . . . . . . . . . . . . . 24, 28 cytokines . ... ... .. . ... .. . . 88
damage, disc . . . . . . . . . . . . . .. . ... 14 damage, nerve .. 14, 46, 49, 56, 60, 61, 66, ... .. ... .. .. . . .. 67, (68), 85, 89 damage, tissue ..... 9, 12, (26), 29, 64, 71, 80, . . . . . . . . . . . . . . . . . . 82, 83, 96, 114, 116 damage, joint. . . . . . . . . . . . . . . . . . . . .. 59 deep learning. . . . 111 depression . . . . . . . . . . . . . . . . . . . . .. 87, 104 diabetes.. .. .. .. .... .. . . . . . . . . . . . . . 28 diagnosis / diagnoses. . . . . . . . . . . .. .. 82, 83 diet . . . . . . . . . . . .. . . . . . . . . . . . . . . 46, 108 disc. .. .... .. ... ... .... . . . . . 84 disc bulge . . . . . . . . . . . . . . . . . . . . . . . . . . . 14 (see also LAFT disc bulge) disease. . . . . ...... 19,28, 60, 71, 94 diabetes. . ...... 28 inflammatory disease (incl. rheumatoid arthritis) . . . ... 49, 58 distributed processing. ........ .. 38, 39 DNA. . . ........ 29, 60 , 62 dorsal horn . . . . . . . .. . . . . 72, 74, (92) dorsal root ganglion (DRG) . 62, 63, 65, . .. ... .. ... . . .. 67, (68) endocrine systems enzymes . . . . . . . . . . evolution. excitatory chemicals
.. 42, 43, 50, .74,78,86, 111 . . . . . . . . . . . 49 . . . . . . . . . . . 98 ... 36, 44, 72, 73
fascia. . . .. .. .. . ... ... . . . . . 49, 57 . 80, 81, 98-102 fear. . . . . . ......... . fibromyalgia. .82,83 flare-up. 105, 115, 116, 117 gangrene gender. glitches God ... graded exposure.
. . .. . ...... . .. . ... 28 ... . ....... 20, 24, 25 .. . ...... . . . . . . . . . . 123 .......... .. ... 25 114-117
headache. . . . . . . . . . . . . . . . . 97, 114 healing / healing behaviours ...... 8, 9, 11, 19 ... . 43,48,47,49,58, (68), .. .. ... .. . .. 70, 71, 82, 87, 91, 100, 110 homuncular / homunculus ..... 23, 56, 57, 76 hormones .... . . . . . . . . . . . . .. . hyperalgesia. hypnosis
.86,87 . . 72 .... . 17
ignition nodes.
. ...... 38, 76, 78, 100, 115, 116, 121 immune system ..... . 43,88,89 impulse .. . . .. .. . .... . . . .. . . . .. 30, 64, 80 inflammation. . . . . . . . . . .48-50, 71, 87 inflammatory soup . . . . . . . . . . .. . .... 49 initiation .. .. .. .. .. .. ... .. ......... 25 inJection .... .. .. .. . .. . . 31, 54 inJury . . . . . 21, 50, 54, 71, 80 internal pain control system. . . 37 itch . . .. .. ... .. . . 67 jOints ..
.88,59
LAFT - living adaptable force transducer (see also disc) . .. ... .. . . . 84, LAFT disc bulge . . . . . . . . . . . . . . . . . . . . . . latency of pain. . . . . ........ leprosy. . .. . . .. . . . . . . . . . . . . . . . . . ligament. . . . . . . . . . . . . . .. . ........ 55, low back pain . . . . . . . . . . .. 11, 14, 55, 80,
88
14 83 28 61 83
management . .. 102, 104, 106, 108 mastectomy .. ...... 20 memory.......... .... . . . . . . . . . . ...84 metaphors. . .... 74, 75, 78 mirror pain . . . . . . . . . . . . . . 89 motor system. . . . . 43 muscle ....... 23, 42, 52, 53, 90, 91, 110, 113 myofascial syndrome. . . . . ..... . ..... 83 nerve ... backfiring .. .. .. . .. .. . .. .. .. .... .. 6 4 pain. . . . . . . .............. . 6 8 peripheral. . . . 60, 63, 66, 67 ulnar. .. .. 60 nervous system central . . . . . . 18, 30, 7 0 , 72, 82, 113 parasympathetic. . .... 43, 78, 84, 85, 88 sympathetic. . . . ... . . . . 43, 85, 88,111 neurone ... . . 30-33, 38-44, 64, 65, 72, 73, 76 . . . . . . . . . . . . . 78, 92, 119, 120, 123 neurotag . .. . 38, 39, 76, 78, 92, 119, 120, 123 nociceptionlnociceptor. . . .... . 32, 59, 97 opioids. . . . . . . . . . . . . . . . . . . . . . 37 orchestra . .. 40-43, 78, 96, 100, 112, 113, 121
129
Further reading pacing .. 114, 116-118, 122 pain behaviour . . . . . . . . . . . . . ....... 24, 97 labour pain . . . . . ..... . . . . . 16, 25 non-specific back ...... 83 non-specific neuropathic . . . . . . . . . . . . . . 83 spreading. . . . . . . . . . . . . . . . . . . . 82 thresholds. . .. 21, 25 peripheral sensitisation. . . . .. 22, 23 phantom pain . . .. . . . 22, 23, 26 protein. . . . . ... .... . 31 psychosomatic pain syndrome . . . . . . . . . . . 83 repetitive strain Injury . 83 rheumatoid arthritis (see inflammatory disease) sensitivity . . . . . . . . . . . . 72, 73 sensitisation . . . . . . . . . 82, 83 sensor. . . . . . . ........ 30-35, 52, 55 sex (see also gender). . . . . . . . . . . . . . 100 skin. ... .. ...... ..17,56,57,61 skull . . . . . ... ... ... . 29, 58, 70 sliders . . . . .. 122 soft tissue. . . . . . . . . . . . . . . . 56, 57 smudging. . .... .. 23, 76, 77 somatoform pain disorder . . . ........ 83 spike . . . . . . . . . . .. . . ..... 34 Spinal cord ...... . 31-34,36,38,39, (44), 48 . 55, 60, 62, 63, 70-72, 74-76 , 82, (92) stress. . . . . . . . . . . . . 42,67,86,89 suffering . . . . . . . . . . . . . . . . . . . . . . . . . . . . 97 surface learning. . . ..... . ........ III surgery. . . .... 17, 22, 46 synapse .36, 37, 40, (44), 72, 73 tennis elbow . . . . . . . . . . . . . . . . . . . . 66 thought viruses. . . . . . . . .80, 81, 91 threat . .. 76, 83, 84, 102 tissue. . . . . . . .. . .... 48 , 55, 56, 68, 74 , ... ... ... .. .83, 88, 113-117, 122 tolerance. . . 25, 116, 117 toothache. . ........ 21 venebra. . ... 29, 54, 55 virtual body. . . . ... 22,23,76,77 . . . 118 , 120 , 122
war .. whiplash work x-ray
. 13 .28 18, 20, 25, 100 .... 14,59,99
There are many books on pain and the neuroscience behind pain, including several aimed at the general public. We have selected 6 books that we think are the best reading and are aimed at both health professionals and lay people. 1. Wall, P.D., Pain, the Science of Suffering. 1999, London: Weidenfield & Nicholson
A beautifully written and challenging book. A must read for clinicians therefore a useful book for pain sufferers . 2. Melzack, R. and P.D. Wall, The Challenge of Pain. 2nd ed. 1996, London: Penguin
The best book for the public wanting to understand the basis of pain. These clinical SCientists wrote the gate control theory. 3. Nicholas, M., et al., Manage your Pain. 2000, Sydney: ABC Books
This self help book was written by the pain management team at Royal North Shore Hospital in Sydney, Australia. 4. Martin, P., The Sickening Mind. 1997, London: Harper-Collins.
A great guide to the biological effects of stress. Pain is of course, a universal stressor. 5. Sapolsky, R.M., Why zebras don't get ulcers: an updated guide to stress, stress-related diseases, and coping. 1998, New York: W.H. Freeman and Co.
Another guide to the biological effects of stress. 6. Shone, N., Coping Successfully with Pain. 1995, London: Sheldon Press.
One man's guide to confronting and overcoming chronic pain .
___ Explain Pain poster collection As you use the book Explain Pain in your clinic or home, you will
find some images and concepts stand out as particularly useful in the recovery journey. The Explain Pain poster collection is designed to help you and your patients take that journey. The posters can be used in a pain peer group setting, in the waiting room of your clinic, or as an educational tool hanging on the clinic wall for everyday use. They will help pain sufferers to make informed choices and guide them to recovery. The four titles encourage empowerment: Take Control, Pacing Activity, Thought Viruses, The Road to Recovery.
Nor Neurodynamics resources
Nor Brain training resources [email protected] Cards A therapeutic resource for upper limb motor control problems. Even simple exercises may cause pain if your brain can't recognise whether you are using your left or right side. This can be tested easily and quickly using the recognise' Flash Cards. These cards may be used on their own, but are best used with the recognise' limb laterality CD. The CD has a large library of both hand and foot images and has tools for tracking and evaluating progress. The Flash Card set consists of forty-eight left and right hand images on sturdy plasticoated card, a texta, instructions for use, reference list and suggestions of games to 'retrain as you play'. English / German
N eurodynamic Techniques DVD & Book
[email protected] laterality CD
NOI's international group of faculties presents the definitive manual of neurodynamic techniques for everyday clinical use. This DVD and handbook will help with the assessment and management of physical health and sensitivity issues related to peripheral and central nervous system pain presentations.
This novel evidence-based program provides a measurable, progressive self-management computer tool for patients with painful hand and foot problems. Patients are presented contextually graded and randomised images to test and treat alterations in the recognition of their limb laterality. Test results can be collected and analysed. This tool can provide valuable help in the management of Repetition Strain Injuries, CRPS and many chronic pain states. English German
NTSC English PAL, Region 0 English with subtitles in German, Italian, Spanish and Chinese Mandarin.
The Sensitive Nervous System This text calls for skilled combined physical and educational contributions to the management of acute and chronic pain states.
~.
It offers a 'big picture' approach using best evidence from basic sciences and outcomes data, with plenty of space for individual clinical expertise and wisdom.
NO! Red Wedge Our wedge is light, strong and allows very localised active and massive mobilisation of joint and neural tissue in the thoracic spine. These techniques are demonstrated in the Neurodynamic Techniques DVD and Handbook and on NOI courses .
NO! Mirror Box Mirrors may be used for a variety of pain and disability states especiallY involving the hands and feet. In particular, mirror therapy may be appropriate for problems such as complex regional pain syndrome, phantom limb pain, stroke and focal dystonia. Many people gain pain relief and better movemeIJ-t by using a mirror. English German I Italian
II
':':1'
-
'~~/' '
t·t ~ .... ..
-'.
',:
••••;~;'!,., ' .
'
;
For online ordering, new products and course information visit:
www.noigroup.com
----------1
Abstract
Chronic pain is a widespread problem in the field of pediatrics. Many interventions to ameliorate pain-related dysfunction have a biobehavioral focus. As treatments for chronic pain (e.g., increased movement) often stand in stark contrast to treatments for an acute injury (e.g., rest), providing a solid rationale for treatment is necessary to gain patient and parent buy-in. Most pain treatment interventions incorporate psychoeducation, or pain neuroscience education (PNE), as an essential component, and in some cases, as a stand-alone approach. The current topical review focuses on the state of pain neuroscience education and its application to pediatric chronic pain. As very little research has examined pain neuroscience education in pediatrics, we aim to describe this emerging area and catalyze further work on this important topic. As the present literature has generally focused on adults with chronic pain, pain neuroscience education merits further attention in the realm of pediatric pain in order to be tailored and implemented in this population.
1. Introduction
Pediatric chronic pain has reached epidemic proportions with an estimated 1.7 million children in the USA alone suffering from moderate to severe persistent pain [1]. With the high number of children affected, it is of extreme importance to discover new, innovative methods of treatment for the pediatric population. One approach that has been researched and implemented in adult populations over the past several decades is psychoeducation, either as one element of a comprehensive treatment program or as a stand-alone intervention. By explaining the scientific concepts that are central to the pathogenesis and perpetuation of chronic pain, clinical providers hope to create lasting change in the patient’s beliefs about pain, and in turn, increase their engagement in the biobehavioral recommendations made for pain management and reduction. Pain education addresses patient misconceptions about physiological phenomena and helps shift their perspective to the idea that pain is dependent on biological, psychological, and social processes. One common message is that pain is dependent on meaning [2], and that how the patient perceives their pain is key to how a patient’s brain processes pain signaling [3]. Taken together, pain education programs center on an explanatory model that understanding pain can modify pain itself.
Several terms have been coined in relation to pain education with each aiming to convey the central idea of a given approach. They include psychoeducation, pain neuroscience education (PNE), pain biology education, therapeutic neuroscience education, and Explain Pain (EP). For simplicity, we will refer to these approaches broadly as pain neuroscience education (PNE) [4], unless describing a study where a specific approach was empirically tested. PNE can be taught as an intervention on its own, as well as in combination with another form of therapy (such as cognitive-behavioral or physical) [5]. Although it is likely that all patients suffering with chronic pain can benefit from a shift in mindset provided via PNE, it might be critical for patients who suffer from a centralized pain problem and/or struggle with maladaptive perceptions about their pain [6]. This paper reviews the current state of the art in pediatric PNE. As most PNE research has been conducted in adult populations to date, we discuss both adult and pediatric studies within each section, considering how adult studies can inform future pediatric research, and presenting next steps for the pediatric pain field.
2. Why Pain Neuroscience Education?
2.1. Contextual Information about Pain Influences Pain Perception
When examining the concept of PNE, it is helpful to look to experimental research to determine the theoretical efficacy of education in altering pain outcomes. When we educate patients about pain, this new information alters the context in which they perceive their pain. In adult non-patient populations, research has demonstrated that manipulation of information and context regarding a stimulus can modulate pain. In one adult study using a cold pressor test (CPT), stimulus information was manipulated by having one group read a threatening passage about frostbite, while another read a passage about the safety of the test and how pain can be unrelated to tissue damage [7]. They found that the group that read the threatening passage had a lower mean pain tolerance time. In another adult study, investigators examined the idea that heat can be perceived to be more tissue-damaging than cold [8]. A −25 °C metal stick was placed on participants’ necks after telling them that it was either hot or cold. Those who were told that the metal bar was hot rated both the painfulness and the damaging properties of the stimulus higher than participants who were told the metal bar was cold. In a third adult study, it was shown that using the colors red and blue as visual cues before presentation of a stimulus modulated pain intensity [9]. A red visual cue indicating heat resulted in higher pain ratings than a blue visual cue indicating cold.
In pediatrics, the manipulation of information and context has also been shown to modulate pain expectations and emotional response to pain. In one study [10], non-patient children completing a CPT received either threatening CPT information (CPT described as very painful, high pain expressions depicted) or non-threatening CPT information (standard CPT instructions provided, low pain expressions depicted). Children in the high-threat condition expected more pain, perceived the pain as more threatening, and catastrophized more about the pain. Parents of children in the high threat condition also expected their child to experience more pain. In another, parent-focused study [11], parents received either threatening information (stimulus described as painful and barely tolerable, high pain expressions depicted) or non-threatening information (stimulus described as slightly unpleasant, low pain expressions depicted) about a heat stimulus their child would receive. Parents who received the threatening information showed stronger negative physiological responses (EMG corrugator activity and fear-potentiated startle reflex) to cues of upcoming child pain. This was particularly the case when the child’s pain facial expression was high, suggesting that parent beliefs are impacted by information from the environment and from the child.
With regards to patient populations, many individuals suffering from chronic pain can develop irrational beliefs and fears (including catastrophizing) about their pain. Many patients believe that their pain is harmful to their bodies and associate it with danger, despite the absence of tissue damage. These associations, similar to a red light visual cue or a passage about the dangers of frostbite, may worsen their pain. In adult patient populations, it has been shown that exposing patients to inaccurate information regarding illness may harm health outcomes and care [12]. Moreover, adult patients who are unsure of the diagnosis of their pain problem or perceive their pain as enduring and mysterious display higher levels of catastrophizing and are less likely to use coping strategies to deal with their pain [13,14].
In pediatrics, qualitative research also indicates a negative impact of diagnostic uncertainty and inaccurate information provision on child and parent pain and medical experiences. Children who are better informed about a forthcoming medical procedure are generally shown to have better outcomes (lower distress and better adjustment) during and after the procedure [15]. For parents, feeling uncertain with regards to their child’s chronic pain condition and prognosis is shown to relate to parental feelings of helplessness and distress [16]. Studies are now needed to directly examine the effects of information provision in pediatric clinical populations. Due to the important role of child and parent beliefs and fears, it is crucial that healthcare professionals assess and appreciate these beliefs in order to determine if PNE would be an appropriate and worthwhile intervention within the context of pediatric pain.
2.2. Pain Neuroscience Education Provides a Common Language between Provider and Patient
A gap in understanding and communication between the patient and doctor can be a barrier in the treatment of chronic pain. PNE may provide a common language to aid communication and understanding. However, doctors’ expectations of patient understanding and actual patient ability to understand must align for patients to receive helpful information about pain. A study with adults used the Neurophysiology of Pain Test to assess the ability of patients and healthcare professionals to accurately understand the neurophysiology of pain, as well as healthcare professionals’ perceptions of the ability of patients to understand the concepts [17]. The results showed that after an education session, both groups were able to understand the information, but healthcare professionals significantly underestimated the ability of patients to do well on the Neurophysiology of Pain Test.
In pediatrics, discrepancies between doctors’ expectations of patient understanding and actual patient ability to understand may be particularly pertinent, as patients’ cognitive capacity changes across development, and does not always align with child age. The effect of age and cognitive capacity on PNE efficacy is currently unknown. However, a 2007 review acknowledged the importance of cognitive-developmental considerations within the provision of information regarding pediatric medical procedures [15]. Research has also indicated communication issues between child chronic pain patients and doctors, as well as discrepancies between doctor information provision and patient needs. The oral testimonies of patients at the Pediatric Pain Clinic at UCLA revealed patient frustration regarding the doctor’s lack of interest in their experience [18]. The testimonies suggested a fundamental difference in the language and orientation of patients and doctors in regards to pain. While the child’s orientation was experiential and emotional, the doctor’s was instructive and diagnostic. This suggests that changes are needed in the communication models employed in treating pediatric chronic pain so that information being exchanged between treatment providers and patients begins to resonate. In addition, if providers assume their patients will not understand pain neuroscience information, they will not attempt to include it in appointments or treatment sessions. Thus, it is necessary for providers to be well-versed in PNE and to feel comfortable delivering that information in a developmentally appropriate way.
3. Overview of Pain Neuroscience Education
3.1. Explanatory Models
There are several theoretical models that have emerged to explain chronic pain, many of which have already been applied to a pediatric population. These models outline the concepts that are the foundation of PNE, provide physicians with a way to conceptualize different aspects of the patient’s pain (including the obstacles that patients must overcome), and offer scaffolding for researchers formulating new research questions. As more information is learned over time about pain, the components of these theoretical models have evolved. Here we describe each model in turn, before presenting their pediatric application, where evident.
Originally, pain was viewed within a biomedical model. This model assumes a one-to-one correspondence between tissue damage, nociceptive input, and pain sensation. Thus, pain was thought to be a direct response to injury, and psychological or behavioural issues were thought to arise as a consequence of pain but not to influence the pain itself [19]. However, by the late 20th century, scientists began to shift away from this idea and moved towards the concept that motivational, affective, and cognitive processes can modulate pain, and can in some cases be the initial factor in pain etiology [20]. This is especially relevant to those suffering from chronic pain, as the pain often emerges despite seemingly normal biological functioning. The biomedical model has now largely been replaced with a biopsychosocial model, which incorporates all of the aspects in a patient’s life that converge and potentially maintain a cycle of pain [21]. This has been determined to be a more effective conceptual and theoretical stance as it is suggested that pain cognitions are not only associated pain intensity, but may also be barriers to effective treatment if left unaddressed [22].
The biopsychosocial model puts an emphasis on the fact that ‘pain itself is modulated by beliefs… and can therefore be improved by modifying inaccurate beliefs’ [2]. In order for this model to be successful, health-care providers need to convey the multi-dimensional causes of pain that are to be tackled in the intervention. The biological component of the biopsychosocial model largely revolves around the complex interplay of several cortical and subcortical brain regions involved in sensory, motor, cognitive, affective, and motivational functions [23]; with recent data suggestive of global brain connectivity reorganization among chronic pain patients [24]. This bombardment of neural input is a key mechanism that leads to chronic pain, as the brain keeps sending pain signals even in the absence of tissue damage. One theory that centers on the psychological aspect of the biopsychosocial model, entitled The “Common Sense Model of Self-Regulation” [25] highlights health beliefs and builds a hierarchical framework of patient cognition [26]. The model details the individual’s representation of a health threat and the factors that contribute to this representation. It describes the way in which a person responds to any given health threat, including cognitive and emotional processes. Five dimensions of these cognitions have been identified and include: (1) identity (the effort to evaluate symptoms and label the illness); (2) cause (the subjectively formulated belief of what is causing the symptoms); (3) time-line (the patient’s perception of how long the problem will last); (4) consequences (the patient’s predictions of how the illness will affect them in different areas of their life); and (5) controllability (the patient’s belief regarding their outcome and personal ability to change it) [2,3,27]. PNE, being closely tied to cognitive-behavioral treatments, shares significant ideology with the Common Sense Model of Self-Regulation. PNE aims to help patients reevaluate their pain problem, to target beliefs in order to develop more effective coping skills, and to ultimately change each of the five cognitive dimensions to achieve a positive outcome. The Common Sense Model has been said to be instrumental in the foundation of many cognitive treatments [26], and has been used in a randomized controlled trial of pain education in adults with cancer [28].
In addition to the comprehensive biopsychosocial model, additional theoretical models have emerged that highlight and attempt to explain in greater detail the different aspects of this larger framework. John D. Loeser has described pain as an onion consisting of four layered components: nociception, pain, suffering, and pain behavior [29] (Figure 1). The lower layers of suffering, pain, and nociception are not visible on the outside, being private experiences that only the patient is subjected to. The exterior of the onion is pain behavior, which is how the individual expresses his/her pain to the public. This could be through words, actions, or expressions. The onion model illustrates that in order to deliver effective treatment, the patient’s hidden layers must be acknowledged and understood.
Loeser’s onion model displaying the four components of pain phenomena. Reprinted from Loeser, J.D. Pain as a Disease [29].
Among several cognitive-affective processes at work in the context of chronic pain, none have received greater research [30] and clinical attention [31] than pain-related fear. This is likely due to the inherently adaptive nature of fear in response to a noxious stimulus. The Fear-Avoidance Model (FAM) [30,32] details the cycle of pain-related fear and activity avoidance that ultimately leads to functional disability. As we adopt a biopsychosocial stance on the persistance of chronic pain, fear is argued to influence patient motivations, decisions, and well-being. For some individuals, breaking a vicious cycle of fear and avoidance will necessitate an extensive and thorough PNE. Through learning new information about the biology of pain, patients may be able to rework their relationship to their pain and change their maladaptive and fearful response to an adaptive and flexible one, eventually leading to a better quality of life [33].
Application of Explanatory Models to Pediatrics
The models described above are often used in pediatric clinical settings [34], although there is little published research presenting adaptations of these models for pediatric delivery. The importance of the biopsychosocial model was highlighted in a recent case study of a nine-year-old girl with functional abdominal pain [35]. In this case, it was explained to the patient that pain does not necessarily require a noxious stimulus and can be modulated by experience and context. By using diagrams and age-appropriate metaphors (Figure 2), the complex scientific topics were put into simpler terms and provided the patient and her family concrete reasoning for her persistent pain state.
Visual representation of the biopsychosocial model in the context of pediatric functional abdominal pain. Adapted from Brown, L.K.; Beattie, R.M.; Tighe, M.P. Practical management of functional abdominal pain in children [35].
The Common Sense Model has also been explored in youth with type 1 diabetes and sickle cell disease, conditions which are often accompanied by frequent pain [36]. However, it has yet to be well applied to other pediatric chronic pain populations. Perhaps the most well-adapted model for pediatric populations is the Fear Avoidance Model (FAM), which has been adapted [37] and validated [38] for youth with chronic pain (Figure 3). In particular, the pediatric FAM considers the important influence of parents for the child pain experience, including parental cognitions, affective responding, and coping behaviors. In a first empirical study, child FA factors were shown to be a good predictor of functional disability in youth with chronic pain [39]. Interestingly, duration of pain contributed to the model for younger children, whereas pain-related fears were more influential for adolescent patients, highlighting the importance of developmental factors in the application of explanatory models to pediatric populations.
The interpersonal fear-avoidance model of chronic pain. Reprinted from Simons, L.; Smith, A.; Kaczynski, K.; Basch, M. Living in fear of your child’s pain: The parent fear of pain questionnaire [38].
3.2. Current Evidence for PNE among Adults
There have been several systematic reviews conducted for adult PNE research that point to potential areas for growth in the field. For example, in 2011 Clarke and colleagues [40] reviewed studies of PNE specifically for chronic low back pain, for which they included only two randomized controlled trials (RCTs). The review revealed very low quality evidence that PNE is beneficial for pain, physical functioning, psychological functioning, and social functioning in this population, although the authors acknowledge that the review was limited by the small number of studies. More recently, Louw and colleagues [41] conducted an additional systematic review with a broader scope. Specifically, they included 13 RCTs that examined the influence of PNE on chronic musculoskeletal pain conditions. Five trials demonstrated positive effects in decreasing pain ratings, while three trials showed no effectiveness. Interestingly, of the three studies that were identified to increase pain knowledge, two of them showed an increase in pain knowledge, as well as a positive effect on pain catastrophization. However, an increase in pain knowledge is yet to be shown to correlate with decreased pain and disability [41].
Overall, the evidence for the effectiveness of PNE in adult patient populations is modest, particularly for long-term outcomes. However, the field is rapidly gaining momentum with additional studies being done each year. Moreover, it may be that the impact of PNE is better measured via its influence on mediators (e.g., pain catastrophizing, fear of pain) that ultimately influence outcomes. Perhaps PNE does not demonstrate a direct impact on pain-related function, but rather exerts its influence via these key mechanisms of change that have a demonstrated impact on outcomes in the literature.
Current Evidence for Pain Neuroscience Education in Pediatrics
To date, there are few studies that examine the utility of PNE in pediatric populations. There is preliminary evidence that psychoeducation may be efficacious for improving pediatric outcomes, however, most studies have investigated educational programs focused on pain management rather than explaining the biology and neuroscience of pain. In 2007, Abram and colleagues [42] randomized pediatric headache patients to receive either a traditional neurological examination only, or the examination alongside a group educational session. The education session comprised information regarding stressors contributing to pain, pharmaceutical and behavioral treatments, and guided relaxation skills practice. Patients receiving the additional educational session demonstrated greater gains in headache knowledge and required slightly less physician face-to-face time. Both groups experienced a sustained decline in headache-related disability. Whilst this study provides preliminary evidence that psychoeducation can increase knowledge about pain management, the study did not examine PNE specifically.
Perhaps unsurprisingly, many Cognitive-Behavioral Therapy (CBT) programs for pediatric chronic pain are delivered within a psychoeducational frame. Interestingly, a small number of RCTs for psychological therapies in pediatric chronic pain have used psychoeducation as a control intervention (see [43]). These studies have typically revealed superiority of psychological therapies (CBT and internet-based self-help training) over education for primary outcomes of functional disability and pain symptoms. However, where information regarding education content was provided [44,45], it is clear that education again focused on pain management rather than PNE specifically. Studies of primary PNE interventions for pediatric populations, particularly with randomized controlled designs, are greatly needed to advance understanding of the efficacy of PNE for pediatric populations.
3.3. New Applications of PNE: Preoperative Preparation and Cancer Pain Treatment
Adult PNE research has rapidly expanded over the past decade, and has branched into new areas such as preoperative preparation and cancer treatment. For example, the Preoperative Neuroscience Education Tool (PNET) targets adult patients undergoing lumbar radiculopathy [46]. The goal of PNET is to reduce post-operative pain levels, catastrophizing, and disability, as well as increase physical performance. Since postoperative rehabilitation is often ineffective in reducing pain levels, preoperative education that addresses pain physiology by using illustrations (Figure 4), metaphors, and explanatory examples has been of recent interest.
Example of illustration used in the PNET program to explain nervous system processes related to persistent pain. Reprinted from Louw, A.; Puentedura, E.J.; Diener, I.; Peoples, R.R. Preoperative therapeutic neuroscience education for lumbar radiculopathy: A single-case fMRI report [47].
Similar to PNET is the program RIDcancerPain (The Representational Intervention to Decrease Cancer Pain), that has been used as part of an RCT among adults with cancer pain [28]. RIDcancerPain aims to address the patient’s current beliefs about pain before changing their perceptions through a one-time educational program that introduces new concepts surrounding pain physiology and coping strategies. Results showed that patients receiving RIDcancerPAIN reported greater decreases in barriers to pain control and greater decreases in pain severity than those in the control group. This study is similar to a previous program on cancer pain management, which showed a moderately positive effect on pain intensity after patients watched an educational video and had an informal discussion with a nurse [48]. Although some elements diverge between palliative care and chronic pain management, the emphasis on doctor interaction and education on pain physiology highlighted in these studies demonstrates where PNE converges across patient populations.
In pediatrics, Chambers and colleagues [49] conducted a randomized trial of a pain education booklet for parents of children undergoing surgery. Parents receiving the pain education booklet, in comparison to those receiving a pain assessment control or no pain education, had fewer concerns about the use of analgesics for children, but there were no group differences in parents’ pain symptom assessments on any of the three days following surgery. Again, the pain education booklet focused on pain management strategies rather than explaining the neuroscience of pain. More recently, Tabrizi and colleagues [50] investigated the use of an anesthesia education booklet to alleviate preoperative anxiety in children ages 8–10 and their parents. Whilst parents and children receiving the education intervention reported reduced preoperative anxiety, similar reductions were seen in a control group receiving routine preoperative preparation without education.
3.4. A Combined Approach of Pain Neuroscience Education and Physiotherapy
It has been suggested that PNE sessions alone may not be sufficient to reach efficacious outcomes. Multiple studies have thus examined the success of combining PNE with physical therapy and exercise [51]. In a recent adult study [52], patients with chronic low back pain (CLBP) (n = 30) underwent two sessions of PNE followed by 12 sessions of aquatic exercise, all in a small group setting. The combination of both approaches resulted in statistically and clinically significant reductions in pain and functional disability when compared to the control group (n = 32) that received only the aquatic exercise sessions. This extends the results of a similar study in adult patients with fibromyalgia (n = 58) where the combination of pool exercise and PNE was found to be more effective than physiotherapy alone [53].
This combined approach is not limited to aquatic exercises. Land-based physiotherapy programs have also been successful. This integrated approach has lowered pain and disability in a recent RCT among adults with CLBP when compared to a control group [54]. While the control group (n = 28) only received advice from their general practitioners, the experimental group (n = 29) had a four-week PNE course that incorporated trunk muscle training and a standardized home-exercise program. Another study (n = 41) was completed shortly after, and investigated the use of group or individual education when used in combination with motor control training [55]. The individual education group showed larger decreases in pain and disability than the control group. A similar program was implemented in Brazil, where patients (n = 79) received one hour of stretching alongside a physiotherapist and one hour of CBT-focused psychoeducation with a nurse and psychologist, weekly for eight weeks [56]. Over the eight weeks, patients’ pain intensity and disability levels significantly decreased. Although the latter study did not contain a control group and should thus be evaluated with caution, these studies highlight that PNE within the realm of a multidisciplinary cognitive-behavioral pain management program may enhance patient treatment in the future.
Not all trials have indicated better results when combining PNE with other treatments compared with PNE alone. For example, one recent study among adult patients with LBP found greater decreases in pain and increases in pain self-efficacy in patients who only received pain biology education (n = 18), compared to those who also received group exercise classes (n = 20) [51]. Although this was an unanticipated finding, the authors suggested that an exercise-only group would be important to tease apart findings in a future study.
Again, pediatric research on the combined effects of PNE and physiotherapy is lacking. However, given promising findings from adult studies, and growing support for the effectiveness of physiotherapy within an interdisciplinary program for treating children with chronic pain [57], research in this area is warranted.
4. Delivery Methods
The way that pain education is delivered and presented to patients may be as important as the content itself. Evaluating patients’ individual needs and capacities for understanding PNE is important for PNE success. This may be especially pertinent in a pediatric setting, where PNE must be adapted to match patients’ cognitive capacities. There are many modalities already in use in both adult and pediatric clinical populations, giving healthcare professionals options in how to engage their patients, and giving patients resources they can utilize outside of a doctor’s office. Below we examine common PNE delivery methods, particularly considering their use in pediatric populations.
4.1. Metaphor
When educating patients about pain, creative ways of explaining biological processes are necessary. This is especially relevant to the pediatric population, where traditional lectures or scientific models may be ineffective. Metaphor or story-telling as a way of discussing pain phenomena can be a helpful tool in PNE. A 2013 randomized controlled trial [58] found that adult chronic pain patients given a book of metaphors and stories to explain pain biology, Painful Yarns [59], had a larger increase in knowledge about pain biology and a larger decrease in pain catastrophizing compared to patients who were given a book about pain management. Interestingly, patients in the metaphor group reported reading an average of 82% of their book, as opposed to 47% for the control group, suggesting that metaphor not only has the potential to alter perceptions, but it is also more engaging than more traditional methods of delivery [58].
One metaphor proposed as a way of conceptualizing the pain problem for both patients and healthcare professionals is the pain puzzle (Figure 5); a visual and conceptual metaphor that identifies the multitude of factors that play into pain (nociception, affect/feelings, cognition/thoughts, and behavior). It can be explained that different individuals may have different pieces of varying sizes that make up their ‘personal pain puzzle’. The pain puzzle has been utilized in pediatric clinical settings for patients with rheumatic disease [60].
The pain puzzle visual metaphor. Reprinted from Rapoff, M.A.; Lindsley, C.B. The pain puzzle: A visual and conceptual metaphor for understanding and treating pain in pediatric rheumatic disease [59].
A recent commentary detailed an extensive collection of metaphors and analogies that have been used by clinicians in multiple pediatric settings (Figure 6) [34]. They focus on four explanatory categories: (1) the difference between acute and chronic pain; (2) pain transmission/spreading; (3) factors that impact pain perception; and (4) pain rehabilitation. These metaphors have been used by numerous professionals to explain pain biology, outline treatment goals, and to help patients reconceptualize the pain problem.
Example metaphors for explaining chronic pain to children. Adapted from Coakley, R.; Schechter, N.L. Chronic pain is like… the clinical use of analogy and metaphor in the treatment of pain in children [34].
4.2. Books
Providing patients with written resources that they can utilize outside of the clinical setting can be an instrumental factor in consolidating their reconceptualization of pain.
4.2.1. Adult Pain Books
Explain Pain and Protectometer: The book Explain Pain [61] is being recognized as an invaluable resource for chronic pain patients and for professionals delivering PNE to patients. The book, written by David Butler and Lorimer Moseley, details many facets of pain biology and pain management. It is written in an approachable and engaging format, and includes illustrations throughout [61]. An education program based on the book was shown to result in lower pain scores at a three-month follow up in a group of fibromyalgia patients compared to patients who received education about activity management [62]. A pilot study also utilized the book in a session treating patients with chronic whiplash, and revealed a significant decrease in disability and an increase in pain thresholds at follow-up [63].
A recently published follow-up book, The Explain Pain Handbook: Protectometer [64], is a patient-targeted handbook with updated information which includes an interactive pain treatment tool. The ‘Protectometer’ is a tool that allows patients to map out their pain on a day-to-day basis and identify stressors and what the authors call ‘DIMS’ (Danger(s) In Me) and ‘SIMS’ (Safety(s) In Me). There is also a ‘Protectometer’ iOS APP available (Figure 7) to build upon the activity in the handbook and to provide patients with a user-friendly way to define their ‘personal pain formula’ [64].
Example diagram of the ‘Protectometer’ tool provided in the available iOS app. Adapted from Protectometer: iOS Application in Appliquette. Available online [73].
Why Do I Hurt: Another recent series of patient education books was written by physical therapist and clinical neuroscientist, Adrianne Louw. Why Do I Hurt? [65] is a basic patient pain neuroscience manual for chronic pain, covering pain biology and nervous system phenomena. The material is accessible for readers not already versed in the science, and includes illustrations, metaphors, and examples. Other books in his PNE series are focused on specific chronic pain problems including Why Pelvic Pain Hurts [66], Your Headache Isn’t All In Your Head [67], Whiplash: An Alarming Message From Your Nerves [68], and more [69,70]. There is also a workbook in the series specifically for PNE providers, Therapeutic Neuroscience Education: Teaching Patients About Pain [71]. This book is unique in that it is geared towards clinicians and focuses on the best ways to explain pain and demonstrate pain biology concepts. Louw has also developed the “Why You Hurt: Therapeutic Neuroscience Education System”, a clinical tool including colorful educational flashcards, teaching cues, pain questionnaire cards, and homework cards, all aimed at facilitating PNE [72]. The system provides an innovative way to help providers execute PNE in clinical settings. Although not written for a pediatric audience, these interactive resources hold great potential for engaging younger patients.
Despite the potential value of these materials to patients, they may not be sufficient to replace in-person PNE. In a group of adult fibromyalgia patients, written education alone did not significantly impact pain catastrophizing or functioning during daily tasks [74]. Even if patients may appreciate receiving written PNE, for it to truly be an agent of change, it may need to be delivered in person to provide an engaging, interactive format, or incorporated into a larger treatment plan that targets multiple elements of the biopsychosocial model [75].
4.2.2. Pediatric Pain Books
There is no book that exclusively focuses on PNE in pediatric pain. However, there are several published books from the past decade that have been directed toward parents of youth with chronic pain, a key audience for PNE. These books comprise multiple sections that often include: PNE, education on treatment options, and an introduction to pain management skills (e.g., relaxation, behavioral activation) that parents can foster in their children. For example, “Conquering Your Child’s Chronic Pain” [76] introduces parents to valuable PNE topics and helpful relaxation and visualization techniques. “Relieve Your Child’s Pain” [77] details ways that parents can reduce stress in the home and properly evaluate their child’s pain, and addresses fears parents may have about their child’s pain problem. More recent contributions include “Managing Your Child’s Chronic Pain” [78], which provides parents with insight on CBT strategies as well as vignettes and stories of patient and family experiences, and “When your child hurts,” [34], which provides extensive PNE (over 30 pages dedicated to “Understanding What Pain is (and is Not)”) along with specific strategies geared toward breaking the cycle of the child’s pain problem. The goal of these books is to provide valuable insight and relief as parents struggle to help their child manage chronic pain. Despite the growth in these resources, there are no published studies that examine their impact on parent and child function in the context of child pain.
4.3. Group Education Models
When considering practical and efficient methods of delivering PNE to patients, group education is a viable option. Group models allow for a more time- and cost-efficient platform to educate patients with similar needs. The RCT by Abram and colleagues [42] described above delivered psychoeducation within a group setting, and revealed some positive effects. A group model of education may be a more efficient way to deliver information to patients instead of incorporating it into individual appointments [42]. In addition to increasing efficiency, group PNE sessions may be advantageous in that they give patients an opportunity to connect with other patients and even learn from others’ experiences. However, it has also been shown that a group model, as opposed to a one-on-one session, may suffer in efficacy [51]. The group model has the potential to prevent patients from asking questions or voicing concerns, and the one-on-one patient-clinician model may be vital for clinicians to assist in a patients’ individual reconceptualization of pain. Moreover, there are several issues to consider in relation to group composition that can potentially impact outcomes, such as size of the group, homogeneity/heterogeneity, and age (see recent review [79]). It is likely that a combination of group and one-on-one sessions may provide increased efficiency in a manner that does not sacrifice the individually tailored care that may be essential for effective pediatric pain treatment.
4.4. Video
When presenting PNE to patients, especially in pediatrics, it is likely important to engage them using multiple modalities to facilitate processing complex and novel information. One approach is the use of short video clips. These videos are likely a familiar platform for patients to explore PNE in their own time and in comfortable home environments. One video, created by the German Pediatric Pain Center (Figure 8), explains pain for patients with migraines. Cartoons are used to explain why some people have migraines, what they mean, and how one can manage them [80]. Another video entitled “Understanding pain in less than 5 min” [81] uses active illustrations to present chronic pain from a biopsychosocial perspective. It is available on YouTube in over ten different languages.
Image obtained from the online video, ‘Migraine: how it works and how to get it under control’ [80].
5. Developmental Considerations and Next Steps
Research examining PNE for pediatric chronic pain is somewhat uncharted territory. Despite the clear relevance of PNE to children and young people, RCTs of PNE programs have typically been conducted with adults, and most RTCs employing psychoeduation in pediatric populations have examined psychoeducation only as part of a broader psychological treatment package and in many cases focus on pain management versus pain neurophysiology. As described above, educational resources that are appropriate for pediatric populations are currently available, such as Explain Pain, The Protectometer [64], and online animated videos. However, given that the neuroscience of pain is complex, resources that align with the child’s current state of cognitive and psychosocial development will be essential. Of particular importance for pediatrics, children who are unwell or highly stressed may also be functioning at lower cognitive levels than they otherwise would [15]. Materials must, therefore, be tailored according to both the child’s cognitive-developmental stage and his/her physical and affective state. Consideration of Piaget’s developmental stages may provide insight into the appropriate adaptation for PNE materials and delivery across early and middle childhood. The review by Jaaniste and colleagues [15] provides an excellent example of how to consider these conceptual stages when providing children with information about forthcoming medical procedures, and these examples could be usefully applied to PNE development. In order to appeal to youth at different developmental stages, resources could also be available in multiple modalities. These may be in the format of written resources, in-person dialogue models, or online animated videos and apps. Metaphors and stories should be further utilized to create specific pediatric educational tools as they provide a format for making complex concepts concrete and accessible. It is also important to consider the changing parent-child relationship across development, and recognition of the impact of parents on child learning and beliefs [82]. Most of the pain books developed for pediatric populations described above are targeted at parents, and this may indeed be an ideal method of PNE transmission for younger patients who frequently look to parents for learning opportunities.
6. Conclusions
PNE is receiving growing interest as an intervention in the field of chronic pain. Its potential application is vast, ranging from preoperative prevention programs to cross-disciplinary chronic pain management programs. Since PNE can be applied to multiple treatment scenarios and delivered by a variety of health professionals, its potential influence on patients is broad. Pain neuroscience education is in the midst of finding its place among a plethora of cognitive-behavioral treatments for chronic pain. A necessary next step is the inclusion of pediatric populations. Rationale for PNE, such as the detriment of irrational beliefs and maintenance of fear-avoidance, are equally relevant for younger patients. Given existing evidence for PNE in adults, this topic deserves more attention in the pediatric realm.
Acknowledgments
This work was supported by a National Institutes of Health grant (R01 HD083270) awarded to L.E.S.
Conflicts of Interest
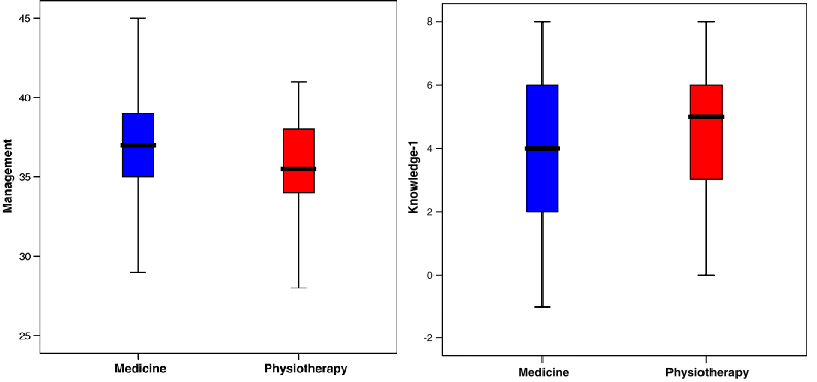
The authors declare no conflicts of interest.